Protein found in patients with severe asthma can help identify who would benefit from targeted drugs
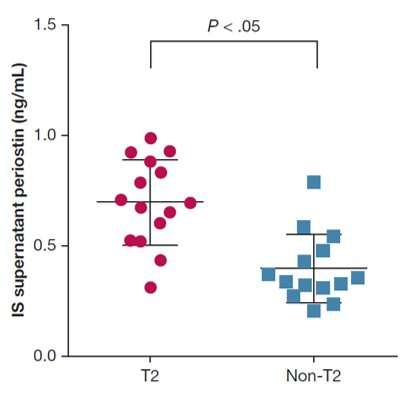
In a novel study, researchers succeeded in identifying patients with a form of severe asthma (type 2 endotype) by measuring periostin concentrations in their airways. These patients with the type 2 (T2) endotype may benefit from newly developed targeted treatments that have the potential to transform their quality of life, report researchers in the journal CHEST.
Asthma can range from very mild with little or no need for medical treatment to severe and life-threatening. Severe asthma is clinically and biologically varied and identifying the specific type of asthma is crucial in targeting patients who will benefit from new treatment options. The role of periostin, a matricellular protein, in asthma and type 2 inflammatory responses, is an area of active research.
"The T2 immunity severe asthma endotype is one of the most consistent endotypes to emerge probably because it is a key driver in nearly half of all patients with asthma," explained Giovanna E. Carpagnano, MD, Ph.D., Institute of Respiratory Diseases, Department of Medical and Surgical Sciences, University of Foggia, Foggia, Italy.
Investigators analyzed periostin concentrations in the airways of severely asthmatic subjects, evaluating the role of periostin in clustering the T2 endotype. They enrolled 40 consecutive severe asthmatic patients (25 asthmatics of T2 and 15 of non-T2 endotype); 21 patients with mild to moderate asthma; and 15 healthy control subjects. All individuals underwent exhaled breath condensate and sputum collection, eosinophil count in blood, fractional 32 exhaled nitric oxide (FeNO) and immunoglobulin E (IgE) measurement. They found that periostin is measurable in the airways and increased in severe asthmatic subjects, especially in those with the T2 endotype.
"There have been several studies about the value of periostin as a marker of severe eosinophilic asthma, but to measure it in blood limits its value as serum periostin derives from several sources outside the lung and can't be considered an organ-specific marker," noted Maria Pia Foschino Barbaro, MD, Institute of Respiratory Diseases, Department of Medical and Surgical Sciences, University of Foggia, Foggia, Italy, who heads the group where the research was conducted.
"Unlike serum periostin, airways periostin is a useful marker of severe eosinophilic asthma and may help to phenotype patients that will respond to the biologic agents," stated senior investigator Peter J. Barnes, MD, DSc, FCCP, of the Airway Disease Section, National Heart and Lung Institute, Imperial College London, UK. "The newly developed biological treatments have the potential to transform the quality of life of patients with T2 severe asthma. This study suggests that airways periostin is the expression of T2 severe asthma and if validated, could be a useful biomarker to apply stratified medicine for severe asthma, and could transform the quality of life of these patients."
"Severe uncontrolled asthma is an expensive disease that accounts for more than 60 percent of the costs associated with the disease," commented Prof. Carpagnano. "The newly developed biological treatments are expensive too, but if directed to the right patients, they will significantly reduce the global cost related to the management of severe asthmatic patients."
More information: Giovanna E. Carpagnano et al, Looking for Airways Periostin in Severe Asthma, Chest (2018). DOI: 10.1016/j.chest.2018.08.1032