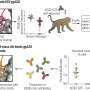
Negligible risk of transmitting HIV during sex when viral load is suppressed
There is a negligible risk of transmitting HIV during sex when a person living with HIV is on antiretroviral therapy and maintains a viral load under a specific threshold, according to a study in CMAJ (Canadian Medical Association Journal).
The systematic review, conducted by the Public Health Agency of Canada, relied on 11 studies and one previously published review to determine the absolute risk of HIV transmission when preventive measures are in place.
"Our findings show that there is a negligible risk of sexually transmitting HIV when an HIV-positive sex partner adheres to antiretroviral therapy and maintains a suppressed viral load of less than 200 copies/mL on consecutive measurements every four to six months. The risk of sexual HIV transmission is low when an HIV-positive sex partner is taking antiretroviral therapy without a suppressed viral load of less than 200 copies/mL, condoms are used or both," writes Rachel Rodin, Centre for Communicable Diseases and Infection Control, Public Health Agency of Canada, with coauthors.
"Based on our findings, relevant case law and other factors, the Department of Justice Canada concluded that the criminal law should not apply to people living with HIV who maintain a suppressed viral load of less than 200 copies/mL." Justice Canada also concluded that the criminal law should generally not apply to those who use condoms, among others.
Previous studies found that antiretroviral therapy and condoms can reduce HIV transmission. This study includes evidence from newer studies that have influenced clinical practice and could affect Canadian criminal law.
"These findings will support individual patient and clinician decision-making, and will have implications for public health case management and contact tracing. The Department of Justice Canada used these findings to inform their 2017 report on the justice system's response to HIV nondisclosure, and they may inform the responses of other justice systems," write the authors.
In a related commentary, Richard Elliott, Canadian HIV/AIDS Legal Network, Toronto, Ontario, also welcomes Justice Canada's conclusions that the criminal law should generally not apply in various circumstances, including cases where condoms are used. However, he cautions that the qualitative descriptions of HIV transmission risk used by the study authors potentially overstate risk as understood in the criminal justice system. "[The study authors'] qualitative assessments of transmission risk apply risk categories originally developed 30 years ago to enable public education about safer sex and health risk reduction in general," Elliott writes. "These categories reflect the relative riskiness of different activities. But they should not be transposed into a system tasked with determining criminal liability based on risk associated with a single act."
Elliott suggests instead that "consensus statements of expert scientific opinion that specifically address the needs of the criminal justice system should guide that system." These support a more limited use of the criminal law than is currently the case in Canada.
More information: Jennifer LeMessurier et al. Risk of sexual transmission of human immunodeficiency virus with antiretroviral therapy, suppressed viral load and condom use: a systematic review, Canadian Medical Association Journal (2018). DOI: 10.1503/cmaj.180311
Richard Elliott. Ending overly broad criminalization of nondisclosure of human immunodeficiency virus infection, Canadian Medical Association Journal (2018). DOI: 10.1503/cmaj.181405