New genetic insight could help treat rare debilitating heart and lung condition

The largest study of genetic variation in patients with pulmonary arterial hypertension has associated two important genes with the disease.
In collaboration with institutes from Europe and Northern America, researchers from Imperial College London have conducted the largest genetic analysis to date of 2,000 patients with pulmonary arterial hypertension (PAH) and identified associations with two genes.
PAH is a rare form of pulmonary hypertension that affects the blood vessels in the lungs, causing high blood pressure that can lead to heart failure. The disease is often fatal and, on average, patients survive 5-6 years after diagnosis. Sufferers feel breathless and tired, with symptoms worsening during exercise.
The research is the first to demonstrate that variations in the SOX17 gene and the HLA-DPB1 gene were associated with PAH. Insight into the genetic mechanisms behind this life-threatening disease could help inform treatments and identify new therapeutic targets.
Common genetic variation
PAH can be related to other conditions such as congenital heart problems, connective tissue disease, and HIV but for many sufferers, PAH is either inherited (HPAH) or arises for no known reason, which is known as idiopathic PAH (IPAH). Around 1,500 people in the UK have either HPAH or IPAH and 10 per cent of sufferers die each year. PAH affects more women than men, typically in their 30s and 40s.
Previous research has identified some of the rare genetic mutations behind inherited PAH, but little is known about the common genetic variation responsible for smaller differences between patients and the variation in their response to treatments. Current treatments include medicines to help prevent blood clots, diuretics and specialist treatments to relax the arteries in the lungs.
Published in The Lancet Respiratory Medicine, the study aggregated data from four international cohorts from Europe and North America on patients with heritable or idiopathic PAH. UK data was from the National Institute for Health Research BioResource (NIHR BioResource) - Rare Diseases and the British Heart Foundation Pulmonary Arterial Hypertension (BHFPAH) study.
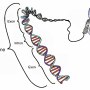
The analysis took a genome-wide association (GWAS) approach, which examined millions of common variants covering the genome. The research identified three genetic signals associated with PAH: two of these were next to the SOX17 gene in the region that 'loops back' to regulate the levels of SOX17 and the third signal was within the HLA-DPB1 gene.
Lead author and British Heart Foundation Intermediate Basic Science Fellow Dr. Christopher Rhodes from Imperial's Department of Medicine, said: "This is the first study at the scale required to look at how common genetic variations influence PAH, which could help us understand variations in how the disease presents itself and how patients respond to treatments.
"We were very lucky to pool data with our collaborators as this has provided us with a large enough sample to study these more subtle genetic variations in a statistically meaningful way. Out of the 23,000 genes in the whole genome we have found that PAH has significant associations with two genes, SOX17 and HLA-DPB1, providing strong evidence that these genes play an important role in PAH. This opens up exciting possibilities for future research into new therapies."
Susceptibility and disease progression
SOX17 is instrumental in the development of the endothelial cells that line the arteries in the lung, indicating it could be associated with the structural changes that make patients susceptible to PAH. Previous research has shown that rare genetic variation in SOX17 can cause heritable PAH.
The other gene identified by the study, HLA-DPB1, is involved in controlling the immune response and plays a role in disease progression. The analysis identified different variations or alleles of HLA-DPB1 within PAH patients and found that the number of years that patients survived after diagnosis depended on which versions were active. About 5 per cent of patients have two copies of the C allele of HLA-DPB1 and on average they survived 13.5 years, whereas the majority of patients (69 per cent) have two copies of the T allele and survived on average 7 years.
One of the variations of HLA-DPB1 identified in the study has also been linked with susceptibility to lung diseases caused by exposure to hard metals such as berylliosis.
Professor Martin Wilkins, a senior author and Head of the Department of Medicine at Imperial College London, said:
"This study represents the enormous efforts of an international collaboration and the generous participation of many patients, making it the largest genetic study of PAH to date. The findings raise the importance of including the genotype as a factor when interpreting the results of clinical studies, as it may be that some patients deteriorate at a rate determined by their genotype, rather than at a rate determined by a new treatment.
"The discovery of a common variant that operates through a gene, SOX17, that is mutated in a few patients with the disease suggests that SOX17 may be more commonly involved in pulmonary hypertension than previously thought. This has implications for the development of new treatments that might come from further work on SOX17."
Professor Metin Avkiran, Associate Medical Director at the British Heart Foundation said:
"PAH is a rare but devastating condition which usually strikes people in the prime of their life.
"This is scientific collaboration at its best. This international team has made real gains in our understanding of PAH by identifying two important genes which contribute to its development, laying the essential groundwork we need to develop new treatments in future."
More information: Christopher J Rhodes et al. Genetic determinants of risk in pulmonary arterial hypertension: international genome-wide association studies and meta-analysis, The Lancet Respiratory Medicine (2018). DOI: 10.1016/S2213-2600(18)30409-0