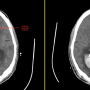
Removing more blood via minimally invasive surgery more likely to improve hemorrhagic stroke recover
The greater the volume of blood removed from the brain via minimally invasive surgery after a cerebral hemorrhage the greater the odds of better functional recovery, according to late breaking science presented at the American Stroke Association's International Stroke Conference 2019.
Minimally Invasive Surgery Plus Alteplase for Intracerebral Hemorrhage Evacuation (MISTIE) is the stereotactic catheter aspiration and clearance of large bleeds within the brain, with the clot-buster alteplase.
The MISTIE III trial is the first surgical trial assessment of whether greater removal of blood impacts the likelihood of favorable functional outcome after one year and factors associated with greater efficiency of blood removal.
Among 506 intracerebral hemorrhage (ICH) cases enrolled in the trial, 242 ICH patients (average age 62, 63 percent male) underwent the MISTIE III surgical procedure by 110 surgeons at 73 sites, with follow-up at one year. The trial excluded patients whose bleeding had not stabilized, and cases with cerebellar and brainstem hemorrhage.
Researchers found that among cases undergoing the MISTIE III surgical procedure, removing blood volume by 70 percent or more, or leaving 15 milliliters or less of residual blood at the end of treatment were twice as likely to achieve milder disability one year later. Lesser removal was needed to avoid mortality, but the patients who had less than 70 percent of the blood removed, or more than 15 mL residual blood, had no difference in disability than patients treated with medical therapy, or those with lesser removal.
Researchers noted that more efficient ICH evacuation was more likely accomplished in cases with certain shapes of hematoma, where the surgical protocol was rigorously followed and by surgeons and sites with greatest experience in MISTIE technique.
"When assessing the results of surgery for brain hemorrhage, it is critical to consider how much blood was successfully evacuated. Unless a large majority of clot is removed and only a very small residual of blood is left, the full benefits of surgery will not be realized," said Issam A. Awad, M.D, M.Sc., study lead author and director of Neurovascular Surgery at the University of Chicago Medicine and Biological Sciences. "This had never been considered as a factor in the success or failure of such surgeries and cannot be taken for granted."
Co-authors and disclosures are noted on the abstract.