How stressed-out bacteria may trigger autoimmune response
Stressful life events most likely contribute to autoimmune diseases, but scientists don't have a deep understanding of the underlying chain of events. A study on mice published this week in mSystems suggests that the gut microbiota may play a significant role in that connection. Researchers found that the onset of stress caused changes in the intestinal bacteria that, in turn, stimulated the activity of immune cells in a way that increased the likelihood that the body would attack itself.
The factors behind autoimmune diseases, conditions in which the body's immune defense attacks its own tissues and systems, can be difficult to pin down. That's partly because these diseases vary in severity and presentation. They include multiple sclerosis, lupus, rheumatoid arthritis, juvenile diabetes, scleroderma, and pulmonary fibrosis. The National Institutes of Health estimates that more than 20 million people in the United States have autoimmune diseases, the vast majority of whom are women.
Although researchers have identified some inherited risks, autoimmune diseases are believed to arise from the complex interplay of genetic and environmental factors. In the study published in mSystems, immunologist Orly Avni, Ph.D., at Bar Ilan University, worked with graduate student Michal Werbner and other collaborators to investigate environmental risks, like psychological and social stress, because those offer opportunities for potential treatment.
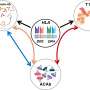
"We know that there's strong crosstalk between the immune system and the microbiota," Avni said. An important step in understanding how stress may lead to autoimmune conditions, she said, is to identify the genetic responses of bacteria. Her group's study showed that social stress changed both the composition and transcriptional patterns in the microbiota. "And the consequent immune response to that threat jeopardized the tolerance to self," she said.
The researchers studied two groups of mice. One was exposed to stress in the form of daily, threatening encounters with other dominant and aggressive mouse. The other group was left alone. After 10 days, the researchers analyzed the gut microbiome of each group and found that the stressed mice had higher levels of some bacteria. Those included Bilophila and Dehalobacterium microbes, genera that have been observed at unusually high abundance in patients with multiple sclerosis.
However, Avni says she's as interested in bacterial behavioral as she is in composition. The study showed that stress led to the activation of bacterial genes related to potentially violent traits—including growth, motility, and signals sent between a pathogen and a host. Microbes with these traits can travel to other parts of the body, including lymph nodes, and elicit an immune response.
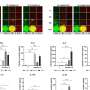
When the researchers analyzed the lymph nodes of stressed mice, they found an increased abundance of several known pathogenic bacterial species. They also found a higher percentage of effector T cells known to play a role in autoimmunity. These findings suggest that stress causes changes in the activity of the gut microbes, which in turn influence the immune response in a way that can eventually trigger an attack of the body.
The study shows that gut bacteria can sense and respond to social stress, but Avni notes that researchers need to better understand how that long-lasting interaction works between bacteria and their hosts.
"It's not enough to study the composition, or the increase or decrease of a species," she said. "We also have to understand how the microbiota sense us, and how they change their 'behavior' accordingly." That knowledge, she added, could potentially lead to tailored microbial interventions that could dampen autoimmunity and additional stress-inducible illness.