Study urges doctors to be on alert for deep vein thrombosis
General practitioners and physicians are being urged to keep a careful eye on the potentially deadly condition of deep vein thrombosis because the signs and symptoms of DVT are non-specific and often difficult to diagnose, according to a review published today in the Medical Journal of Australia.
The review, co-authored by The University of Western Australia's Professor Graeme Hankey, found that clinical presentation of DVT was often "non-specific" and accurate diagnosis required careful integration of clinical assessment, evaluation of pre-test probability and objective diagnostic testing.
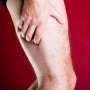
Professor Hankey, a world-leading expert on stroke research, said signs and symptoms of DVT included localized pain, swelling, redness and dilated veins close to the surface of the skin.
The researchers said anticoagulation remained the gold standard treatment for DVT.
"The choice of anticoagulant should consider medical issues such as efficacy, safety, renal and hepatic function, and concurrent medications," Professor Hankey said.
"In addition, practical issues such as availability, familiarity of use, patient preference and cost should be considered."
Compression stockings have been shown to have a beneficial effect after diagnosis. In rare cases, devices to stop blood clots, treatment to dissolve blood clots or surgery to remove blood clots may be considered.
Situations which are likely to impact the choice of anticoagulant agent and duration of treatment include DVT which occurs in pregnant women, patients with cancer, DVT of the lower leg, recurrent DVT, autoimmune disorders such as antiphospholipid syndrome or those with superficial vein thrombosis, Professor Hankey said.
"The diagnosis of DVT requires a high index of suspicion because symptoms and signs are often non-specific," he said. "Anticoagulation continues to be the cornerstone of therapy. The optimal anticoagulant and duration of therapy are determined by the clinical assessment."
More information: Paul C Kruger et al. Deep vein thrombosis: update on diagnosis and management, Medical Journal of Australia (2019). DOI: 10.5694/mja2.50201