Scientists show drug may greatly improve cancer immunotherapy success
A study led by the University of Southampton, funded by Cancer Research UK, has shown a new drug—originally developed to tackle the scarring of organ tissue—could help to significantly improve the success rate of cancer immunotherapy treatment.
Scientists have shown in mouse cancers, that GKT137831 (Setanaxib) can help break down the 'barrier' which makes many cancerous tumors resistant to immunotherapy drugs. GKT137831 is a drug currently undergoing clinical trials for treatment of organ fibrosis.
The team's findings are published in the journal Cancer Research, a journal of the American Association for Cancer Research.
Immunotherapy treatment harnesses the power of the body's own immune system to fight cancer. Its success depends on 'killer' lymphocytes penetrating into a tumor to combat malignant cells. However, most patients fail to respond, often because the lymphocytes are blocked at the edge of the tumor, preventing their attack. The scientists behind this latest study believe they have found why this happens and identified a way to overcome it—potentially improving immunotherapy treatment for many patients with different types of cancer.
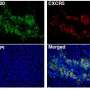
The team found that normal cells called cancer-associated fibroblasts (CAF) are hijacked by cancer cells to protect them from immune attack. Fibroblasts are healthy cells that normally maintain the structure of tissues, but when they are corrupted by cancer cells, they become CAFs and shield tumors from lymphocyte attack and stop immunotherapy from working effectively. A significant proportion of many solid cancers are CAF-rich and associated with poor survival, including more than 50 percent of cases of head and neck, esophageal, colorectal and pancreatic cancers.
Previously, the group had identified that CAF formation depends on an enzyme called NOX4. In this study, they found that blocking NOX4 in mouse cancers, either genetically or with the drug GKT137831, could prevent and reverse CAF formation, allowing lymphocytes to infiltrate tumors and kill cancer cells. Combining immunotherapies with GKT137831 was effective in treating tumors that were previously resistant, significantly improving survival.
The findings could form the basis for making cancers respond better to existing immunotherapy drugs and demonstrate the potential for greatly improved clinical outcomes in a significant number of cancers. Cancer Research UK is currently funding the Southampton scientists to see if this approach improves immunotherapy in breast cancer.
Study author Professor Gareth Thomas, of the University of Southampton's Centre for Cancer Immunology, comments: "Immunotherapy for cancer has been a very exciting development, but still doesn't work in most patients. Our results suggest that in many cases, treatment resistance is caused by CAF, and we think this can be overcome by targeting NOX4. GKT137831 hasn't yet been tested on cancer patients, but we hope may give immunotherapy drugs a much better chance of fighting cancer cells effectively; this technique could hugely improve the success rate of cancer immunotherapy."
Liz Allaway, from Cancer Research UK says: "Immunotherapy is a promising cancer treatment that boosts the power of the body's immune system against cancer, but unfortunately it doesn't work for everyone. This exciting study showed that a drug, currently being tested for the treatment of another disease could make tumors in the lab more sensitive to immunotherapy. The next step would be to see if the drug has the same effect in people, which would open up immunotherapy as a treatment option for more people with cancer."
Ongoing work with Cancer Research UK will now investigate how best to progress these findings.
More information: Kirsty Ford et al. NOX4 inhibition potentiates immunotherapy by overcoming cancer-associated fibroblast-mediated CD8 T-cell exclusion from tumours, Cancer Research (2020). DOI: 10.1158/0008-5472.CAN-19-3158