An accelerated COVID-19 vaccine? Not so fast
Despite headlines suggesting a COVID-19 vaccine might be coming soon, experts at Rice University's Baker Institute of Public Policy warn that a viable vaccine is likely at least a year away.
Insights into the development process were offered during a May 28 webinar featuring Rekha Lakshmanan, contributing expert at the institute's Center for Health and Biosciences and director of public policy at The Immunization Partnership (TIP) in Houston, and Peter Hotez, fellow in disease and poverty at the Baker Institute and dean of the National School of Tropical Medicine at Baylor College of Medicine.
"We're not going to have a vaccine by the end of the year or in weeks or months," said Hotez, whose lab is trying to develop a low-cost vaccine. "And unfortunately a lot of the imagery and language around these processes have created a lot of confusion."
Hotez said when a biotech company, for instance, says it will have a vaccine in weeks, what it really means is the vaccine can be manufactured or produced that quickly at small scale.
Vaccine candidates go through rigorous and layered testing, and Hotez and Lakshmanan said most of them fail—about 90%. By testing multiple candidates, scientists have a better shot at finding one that is safe and effective. They estimate it will take at least a year, maybe longer, to collect enough data showing a potential vaccine's efficacy.
"Vaccines go through a very time-intensive and rigorous scientific process before a vaccine even becomes available to the public," Lakshmanan said. "And from a time context it can take anywhere from 10 to 15 years, sometimes even more, to study and research a vaccine candidate and then make it available to the general population. Even though we have vaccines that go through this trialing process, there's no guarantee or assurances that were actually going to get a viable vaccine candidate out of all these trials."
Lakshmanan said few vaccine candidates make it past the preclinical phase, during which studies are conducted using human tissue or cell cultures or animals to assess the safety of a vaccine candidate.
If a potential vaccine passes that initial test, it must then go through three additional phases. The first includes giving the vaccine to a small group of volunteers, about 20 to 100 healthy adults, to ascertain safety, immunity response and potential dosage. Phase two increases the group size and includes additional populations, such as older adults, and new queries about side effects and individual responses to the vaccine. Phase three is a similar test conducted on a much larger number of volunteers, sometimes into the thousands, which may uncover side effects that previously had not been evident.
If a vaccine candidate clears those hurdles, it may then go to the Food and Drug Administration for review.
According to Lakshmanan, most COVID-19 vaccine candidates are currently in phase one. At this rate, Hotez said, a viable vaccine likely won't be available until next fall—"and even that would be a world record."
"There's a lot of confusion about what's really going to happen in what we're hearing from the pharma companies and even statements coming from the White House coronavirus task force," Hotez said. "Here's what's happening: There's going to be at least seven or eight or as many as 15 or 20 candidates that go into clinical trials. And hopefully ours, our vaccine that we've developed at National School of Tropical Medicine at Baylor College of Medicine and Texas Children's (Hospital), will be one of them."
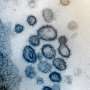
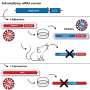
A successful COVID-19 vaccine will function by "inducing an immune reponse to the spike protein of the virus—the spike protein is what binds to the host receptor," Hotez said. "All antibodies work by introducing antibodies to the virus to neutralize the virus, to prevent it from binding to the host tissues."
The spike protein can be genetically engineered by putting its gene in an "expression vector" such as yeast and letting it ferment—"just like you make a beer," Hotez said. Instead of alcohol, the yeast will release a "recombinant protein."
Hotez and his team are using this type of protein in their vaccine candidate. They used a similar process for a SARS vaccine and are hopeful the process could be effective against COVID-19; both diseases are caused by coronaviruses.
"We can know that our recombinant protein vaccines, and some of the inactivated vaccines, give really high titers of neutralizing antibodies," Hotez said. "The other ones haven't."
Other competitors are using DNA or messenger RNA vaccine technology to help get candidates to trial quickly, but Hotez said these types of vaccines are not the best for inducing a certain type of neutralizing antibody required to combat the coronavirus. The neutralizing antibody binds to the spike protein of the virus and blocks it from invading the host's cells.
"Developing a COVID-19 vaccine may not be all that complicated," Hotez said. "It's a straightforward problem in it's (an) old-school biology problem. You need to induce lots of neutralizing antibodies, and we know how to do this."
Hotez said there are ways to accelerate the process of getting a safe and effective vaccine to the public—including manufacturing candidates at a large scale from the beginning of trials so they will be available to the general population if they're successful—and that doing so for COVID-19 could provide a framework for addressing future disease outbreaks.
"If all of this works and the stars align and we do have a vaccine at the other end in say a year and a half from now, that may change the way we think about doing vaccine development going forward," he said. "Because we will have other pandemics and other epidemic threats."