US revokes emergency use of malaria drugs vs. coronavirus
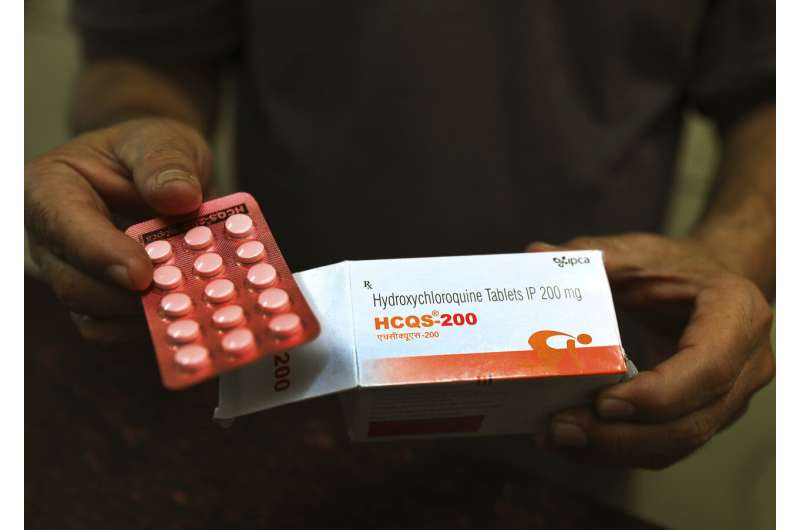
U.S. regulators on Monday revoked emergency authorization for malaria drugs promoted by President Donald Trump for treating COVID-19 amid growing evidence they don't work and could cause serious side effects.
The Food and Drug Administration said the drugs hydroxychloroquine and chloroquine are unlikely to be effective in treating the coronavirus. Citing reports of heart complications, the FDA said the drugs' unproven benefits "do not outweigh the known and potential risks."
In a separate announcement, the FDA also warned doctors against prescribing the drugs in combination with remdesivir, the lone drug currently shown to help patients with COVID-19. The FDA said the anti-malaria drugs can reduce the effectiveness of remdesivir, which FDA cleared for emergency use in May.
Hydroxychloroquine and chloroquine are frequently prescribed for lupus and rheumatoid arthritis, and can cause heart rhythm problems, severely low blood pressure and muscle or nerve damage. The agency reported Monday that it had received nearly 390 reports of complications with the drugs, including more than 100 involving serious heart problems. Such reports represent an incomplete snapshot of complications with the drugs because many side effects go unreported.
FDA's move means that shipments of the drugs obtained by the federal government will no longer be distributed to state and local health authorities for use against the coronavirus. The decades-old drugs are still available for alternate FDA-approved uses, so U.S. doctors could still prescribe them for COVID-19—a practice known as off-label prescribing.
Dr. Steven Nissen, a Cleveland Clinic researcher who has been a frequent FDA adviser, agreed with the decision and said he would not have granted emergency access in the first place.
"There has never been any high-quality evidence suggesting that hyrdoxychloroquine is effective" for treating or preventing coronavirus infection, he said, but there is evidence of serious side effects.
On Thursday, a National Institutes of Health panel of experts revised its recommendations to specifically recommend against the drug's use except in formal studies, and "that, I'm sure, had influence on the FDA," Nissen said.
The actions by FDA and NIH send a clear signal to health professionals against prescribing the drugs for coronavirus.
Trump aggressively pushed hydroxychloroquine beginning in the first weeks of the outbreak and stunned medical professionals when he revealed he had taken the drug preemptively against infection. After Trump's repeated promotions, prescriptions for hydroxychloroquine soared, contributing to shortages.
No large, rigorous studies have found the drugs safe or effective for preventing or treating COVID-19. And a string of recent studies made clear they could do more harm than good.
Dr. Peter Lurie, a former FDA associate commissioner and an Obama administration appointee, said the agency had tarnished its reputation by clearing the drugs based on scant evidence and under apparent political pressure.
"This is an agency that gains its credibility from the strength of its scientific pronouncements," said Lurie, now president of the nonprofit Center for Science in the Public Interest. "The lesson of this whole tawdry episode is that it's the old, painstaking ways of science that ultimately deliver safe and effective therapies."
The only remaining drug with FDA authorization against COVID-19 is remdesivir, an intravenous medication from Gilead Sciences that has been shown to help severely ill, hospitalized patients recover faster.
Late Monday afternoon, the FDA announced it would update remdesivir's prescribing label to warn against combining it with hydroxychloroquine or chloroquine. The agency said results from laboratory tests suggest the drugs interfere with remdesivir's virus-fighting ability in human cells. Despite that risk, regulators said they have not yet seen the problem in patients.
The FDA granted emergency use for the anti-malaria drugs in late March at the same time the U.S. government accepted 30 million doses of hydroxychloroquine and chloroquine that had been donated by two foreign drug manufacturers. Millions of those doses were shipped to U.S. hospitals to treat patient who weren't enrolled in clinical trials.
But the FDA previously warned doctors that it had seen reports of dangerous side effects and heart problems reported to poison control centers and other health systems.
The agency said it revoked the authorization in consultation with the Biomedical Advanced Research and Development Authority, or BARDA, which had requested the emergency use.
BARDA's former director said in April that he was removed from his job because he resisted political pressure from Trump appointees to allow widespread use of the malaria drugs. Rick Bright said he worked with FDA senior staff to limit the drugs' authorization to patients hospitalized with COVID-19 and under professional supervision.
Among other issues, Bright objected to the fact that some of the doses imported were manufactured at facilities in India and Pakistan that had not been inspected by the FDA. Bright is seeking reinstatement to his position at BARDA after being transferred to the NIH.
The FDA says it sampled and tested the imported drugs to confirm they met the agency's standards for safety and quality.
© 2020 The Associated Press. All rights reserved. This material may not be published, broadcast, rewritten or redistributed without permission.