Signaling switch in pancreatic beta-cells determines anti-diabetic drug effectiveness
An international research group has clarified the action mechanism of incretin-based drugs in the treatment of diabetes. The research group headed by Professor Seino Susumu included Researcher Okechi Oduori et al. (Division of Molecular and Metabolic Medicine, Kobe University Graduate School of Medicine), Professor Shimomura Kenju (Fukushima Medical University), Professor Patrik Rorsman (University of Oxford, UK/University of Gothenburg, Sweden), and their teams.
Incretin-based drugs are used worldwide in the treatment of diabetes and in Japan they are currently prescribed to 70% of diabetic patients. However, the mechanism by which incretin-based drugs improve blood glucose levels has been poorly understood.
The findings of the study were published online in the American Scientific Journal Journal of Clinical Investigation on November 16, 2020. A commentary on this paper by Professor Colin G. Nichols and his colleagues at Washington University, St Louis, has also been published.
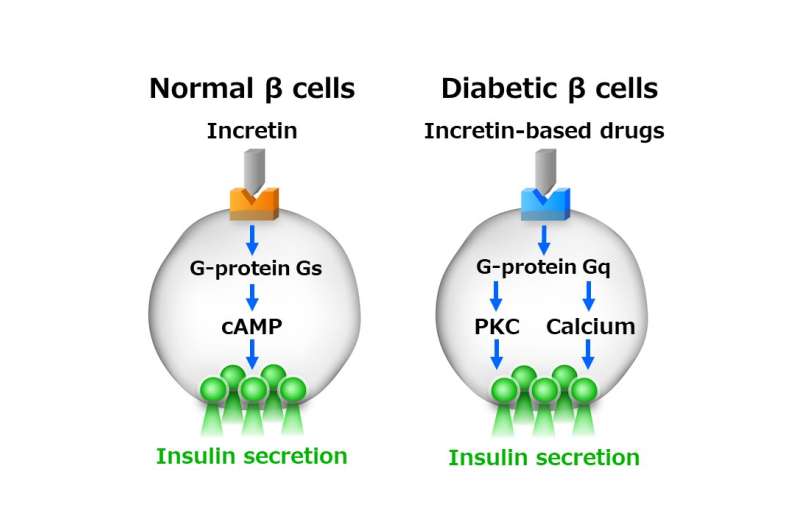
This study revealed for the first time that Gs, a major G-protein signal in normal pancreatic β-cells, is switched to another G-protein signal Gq in the diabetic β-cells to promote insulin secretion, and that incretin-based drugs act on this Gq to promote insulin secretion, thereby improving blood glucose levels.
Research Findings
Incretins are the gut hormones that are secreted by enteroendocrine cells after meal ingestion. The most important function of incretins is to promote insulin secretion from pancreatic β cells. GLP-1 and GIP are known as incretins. While both GLP-1 and GIP are required to maintain normal blood glucose levels in healthy subjects, incretins in patients with type-2 diabetes (T2D) don't function properly. To improve incretin action, incretin-based drugs are used for the treatment of T2D. However, the reason why these drugs are effective has remained unknown.
This research investigated the mechanism of insulin secretion by G-protein signaling in normal β cells and diabetic β cells. Until now, it has been well accepted that the G protein Gs functions as a major signal that promotes insulin secretion in normal β cells. The research group revealed that in diabetes, there is a switch from Gs to Gq signaling in the pancreatic β cells due to continuous β cell excitation. Furthermore, the group discovered that incretin-based drugs act on Gq to amplify insulin secretion, thus improving blood glucose levels.
The Significance of this Research
The results of this research are important not only for illuminating the mechanism behind diabetes, but for diabetes therapies. They might also provide a basis for the development of new treatments.
More information: Okechi S. Oduori et al. Gs/Gq signaling switch in β cells defines incretin effectiveness in diabetes, Journal of Clinical Investigation (2020). DOI: 10.1172/JCI140046