New study reveals extent of brain complications in children with COVID-19
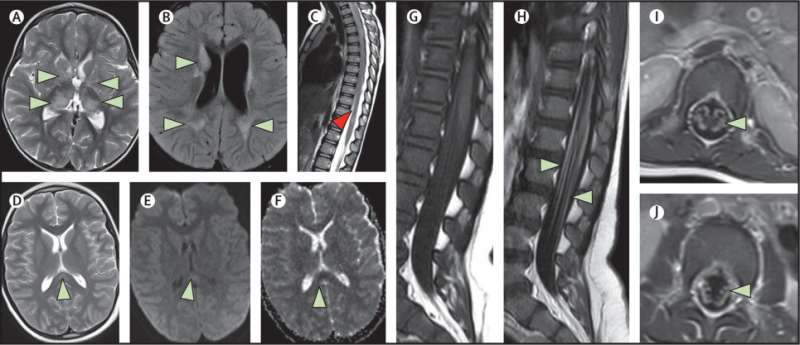
Although the risk of a child being admitted to hospital due to COVID-19 is small, a new UK study has found that around 1 in 20 of children hospitalized with COVID-19 develop brain or nerve complications linked to the viral infection.
The research, published in The Lancet Child and Adolescent Health and led by the University of Liverpool, identifies a wide spectrum of neurological complications in children and suggests they may be more common than in adults admitted with COVID-19.
While neurological problems have been reported in children with the newly described post-COVID condition pediatric inflammatory multisystem syndrome temporally associated with SARS-CoV-2 (PIMS-TS), the capacity of COVID-19 to cause a broad range of nervous system complications in children has been under-recognized.
To address this, the CoroNerve Studies Group, a collaboration between the universities of Liverpool, Newcastle, Southampton and UCL, developed a real-time UK-wide notification system in partnership with the British Pediatric Neurology Association.
Between April 2020 and January 2021, they identified 52 cases of children less than 18 years old with neurological complications among 1,334 children hospitalized with COVID-19, giving an estimated prevalence of 3.8%. This compares to an estimated prevalence of 0.9% in adults admitted with COVID-19.
Eight (15%) children presenting with neurological features did not have COVID-19 symptoms although the virus was detected by PCR, underscoring the importance of screening children with acute neurological disorders for the virus.
Ethnicity was found to be a risk factor, over two thirds of children being of Black or Asian background.
For the first time, the study identified key differences between those with PIMS-TS versus those with non-PIMS-TS neurological complications. The 25 children (48%) diagnosed with PIMS-TS displayed multiple neurological features including encephalopathy, stroke, behavioral change, and hallucinations; they were more likely to require intensive care. Conversely, the non-PIMS-TS 27 (52%) children had a primary neurological disorder such as prolonged seizures, encephalitis (brain inflammation), Guillain-Barré syndrome and psychosis. In almost half of these cases, this was a recognized post-infectious neuro-immune disorder, compared to just one child in the PIMS-TS group, suggesting that different immune mechanisms are at work.
Short-term outcomes were apparently good in two thirds (65%) although a third (33%) had some degree of disability and one child died at the time of follow-up. However, the impacts on the developing brain and longer-term consequences are not yet known.
First author Dr. Stephen Ray, a Wellcome Trust clinical fellow and pediatrician at the University of Liverpool said: "The risk of a child being admitted to hospital due to COVID-19 is small, but among those hospitalized, brain and nerve complications occur in almost 4%. Our nationwide study confirms that children with the novel post-infection hyper-inflammatory syndrome PIMS-TS can have brain and nerve problems; but we have also identified a wide spectrum of neurological disorders in children due to COVID-19 who didn't have PIMS-TS. These were often due to the child's immune response after COVID-19 infection."
Joint senior-author Dr. Rachel Kneen, a Consultant Pediatric Neurologist at Alder Hey Children's NHS Foundation Trust and honorary clinical Senior Lecturer at the University of Liverpool said: "Many of the children identified were very unwell. Whilst they had a low risk of death, half needed intensive care support and a third had neurological disability identified. Many were given complex medication and treatments, often aimed at controlling their own immune system. We need to follow these children up to understand the impact in the long term."
Joint senior-author Dr. Benedict Michael, a senior clinician scientist and MRC Fellow at the University of Liverpool said: "Now we appreciate the capacity for COVID-19 to cause a wide range of brain complications in those children who are hospitalized with this disease, with the potential to cause life-long disability, we desperately need research to understand the immune mechanisms which drive this. Most importantly- How do we identify those children at risk and how should we treat them to prevent lasting brain injury? We are so pleased that the UK government has funded our COVID-CNS study to understand exactly these questions so that we can help inform doctors to better recognize and treat these children."
"Neurological manifestations of COVID-19 infection in UK hospitalized children and adolescents: a prospective national cohort study" is published in The Lancet Child and Adolescent Health.
More information: Stephen T J Ray et al, Neurological manifestations of SARS-CoV-2 infection in hospitalised children and adolescents in the UK: a prospective national cohort study, The Lancet Child & Adolescent Health (2021). DOI: 10.1016/S2352-4642(21)00193-0