Study: COVID vaccine effectiveness declines after 6 months without boosters
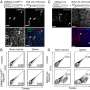
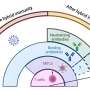
A study released in The Lancet Respiratory Medicine by Providence, one of the largest health systems in the United States, confirms the overall effectiveness of vaccines in preventing severe infection resulting in hospitalization from COVID-19, but also shows a substantial decline in protection after six months. Completed by a team of clinicians and scientists in the Providence Research Network, the study examined data from nearly 50,000 hospital admissions between April and November of 2021, finding that vaccines were 94% effective at preventing hospitalization 50-100 days after receiving the shot but fell to 80.4% 200-250 days later, with even more rapid declines after 250 days.
In addition to examining the effectiveness of vaccines over time, the Providence study was also able to identify factors associated with reduced vaccine effectiveness. Key risk factors for a severe "breakthrough" infection included advanced age (80+), comorbidities such as cancer, transplants, chronic kidney disease, hypertension, or heart failure, the amount of time that had elapsed since being vaccinated, and the type of vaccine one received. For the latter factor, the study found that the Moderna vaccine offered the best overall protection over time, while the Pfizer-BioNTech vaccine offered initial protection equivalent to Moderna's but declined more rapidly over time. Persons receiving the Janssen vaccine also had higher odds of experiencing a severe breakthrough infection compared to Moderna.
"This data helps us understand differences in waning protection by vaccine type and identify the key risk factors for severe breakthrough infections to help inform the targeting of potential vaccine booster programs," said Amy Compton-Phillips, M.D., Providence chief clinical officer. "Unlike most other studies, our data stretched beyond six months, where we found evidence of rapidly waning protection, especially for patients 80 or older. We were also able to identify important differences by vaccine type and patient characteristics that should help inform potential booster programs."
The Providence study, one of the largest of its type, showcases the value of connecting a network of researchers with large scale health care data to help health systems, public health agencies, policymakers, and patients and community members learn and react more quickly to emergent or endemic health challenges. Overall, the data supports the importance of vaccinations for protection against hospitalization, and also clearly evidences the need to boost that protection after 200 days, particularly for patients age 80 and up or with specific medical conditions that increase their risk of severe infection.
"Additional protection may be warranted for everyone, but especially for these populations," said Ari Robiscek, M.D., Providence chief medical analytics officer. "In addition to promoting general vaccine uptake, clinicians and policy makers should consider prioritizing booster shots toward those most at risk for severe COVID-19."
More information: Bill J Wright et al, Comparative vaccine effectiveness against severe COVID-19 over time in US hospital administrative data: a case-control study, The Lancet Respiratory Medicine (2022). DOI: 10.1016/S2213-2600(22)00042-X