Discovery of an immune escape mechanism promoting Listeria infection of the central nervous system
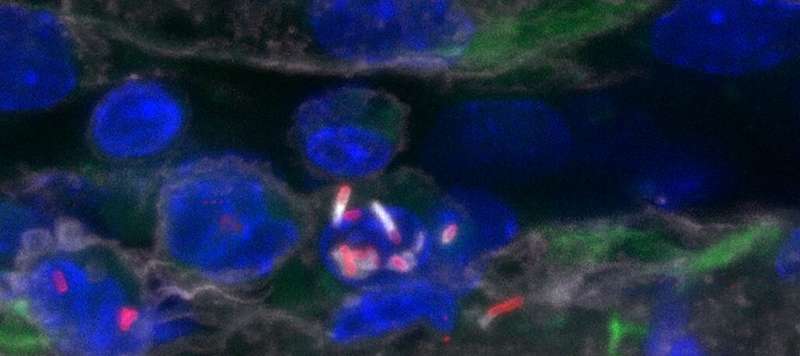
Some hypervirulent strains of Listeria monocytogenes have a greater capacity to infect the central nervous system. Scientists from the Institut Pasteur, Université Paris Cité, Inserm and the Paris Public Hospital Network (AP-HP) have discovered a mechanism that enables cells infected with Listeria monocytogenes to escape immune responses. This mechanism provides infected cells circulating in the blood with a higher probability of adhering to and infecting cells of cerebral vessels, thereby enabling bacteria to cross the blood-brain barrier and infect the brain. The study will be published in Nature on March 16, 2022.
The central nervous system is separated from the bloodstream by a physiological barrier known as the blood-brain barrier, which is very tight. But some pathogens manage to cross it and are therefore able to infect the central nervous system, using mechanisms that are not yet well understood.
Listeria monocytogenes is the bacterium responsible for human listeriosis, a severe foodborne illness that can lead to a central nervous system infection known as neurolisteriosis. This central nervous system infection is particularly serious, proving fatal in 30% of cases.
Scientists from the Biology of Infection Unit at the Institut Pasteur (Université Paris Cité, Inserm) and the Listeria National Reference Center and WHO Collaborating Center led by Marc Lecuit (Université Paris Cité and Necker-Enfants Malades Hospital (AP-HP)) recently discovered the mechanism by which Listeria monocytogenes infects the central nervous system. They developed a clinically relevant experimental model that reproduces the different stages of human listeriosis, and involves virulent strains of Listeria isolated from patients with neurolisteriosis.
The scientists first observed that inflammatory monocytes, a type of white blood cell, are infected by the bacteria. These infected monocytes circulate in the bloodstream and adhere to the cerebral vessels' cells, allowing Listeria to infect the brain tissue.
The research team then demonstrated that InIB, a Listeria monocytogenes surface protein, enables the bacteria to evade the immune system and survive in the protective niche provided by the infected monocytes. The interaction between InlB and its cellular receptor c-Met blocks the cell death mediated by cytotoxic T lymphocytes, which specifically target Listeria-infected cells. InIB therefore enables infected cells to survive cytotoxic T lymphocytes.
This mechanism extends the life span of infected cells, raising the number of infected monocytes in the blood and facilitating bacterial spread to host tissues, including the brain. It also favors the persistence of Listeria in the gut tissue, its fecal excretion and transmission back to the environment.
"We discovered a specific, unexpected mechanism by which a pathogen increases the life span of the cells it infects by specifically blocking an immune system function that is crucial for controlling infection," explains Marc Lecuit (Université Paris Cité and Necker-Enfants Malades Hospital (AP-HP)), head of the Biology of Infection Unit at the Institut Pasteur (Université Paris Cité, Inserm).
It is possible that other intracellular pathogens such as Toxoplasma gondii and Mycobacterium tuberculosis use similar mechanisms to infect the brain. Identifying and understanding the immune escape mechanisms of infected cells could give rise to new therapeutic strategies to prevent infection and also pave the way for new immunosuppressive approaches for organ transplantation.
More information: Marc Lecuit, Bacterial inhibition of Fas-mediated killing promotes neuroinvasion and persistence, Nature (2022). DOI: 10.1038/s41586-022-04505-7. www.nature.com/articles/s41586-022-04505-7