Chronic obstructive pulmonary disease causes premature aging of the immune system, study suggests

A study conducted at the University of São Paulo's Medical School (FM-USP) in Brazil, with results reported in an article published in the journal Immunity & Ageing, shows that chronic obstructive pulmonary disease (COPD) leads to premature senescence (age-related impairment) of the immune system. The finding may help explain why COPD patients respond poorly to vaccines and are more susceptible to infectious processes.
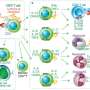
COPD patients were found to exhibit a number of changes linked to immunosenescence, especially a reduction in CD4+ and CD8+ T cells, which are key elements of the immune system.
The study involved 92 individuals divided into four groups: COPD patients (21), smokers without evidence of lung disease (22), healthy older subjects (29), and young adults (20). After analyzing blood samples from all four groups to detect seven markers associated with late differentiation, senescence and exhaustion of immune system cells for each of these groups, the researchers concluded that the COPD patients had cells expressing all the markers in question and that this configured premature aging of the immune system.
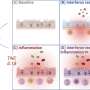
COPD is a chronic inflammatory disease characterized by progressive airflow obstruction and is commonly induced by cigarette smoke and atmospheric pollution. It affects some 64 million people worldwide, according to the World Health Organization (WHO), including about 6 million in Brazil, where smokers or ex-smokers account for 60% of cases.
"As the population ages, understanding the mechanisms involved in immunosenescence is important for several reasons. Knowing how to treat older people, with their increased vulnerability to cancer and infections, and weaker response to vaccines, can help us find better ways to improve the efficiency of the immune system. This study provides additional information on what happens and on the possible interventions," said Gil Benard, last author of the article. Benard is a professor at FM-USP and a researcher in its Dermatology and Immunodeficiency Laboratory. The study was supported by FAPESP.
According to Juliana Ruiz Fernandes, first author of the article, analysis of blood samples from the COPD patients in the study showed faster senescence of T cells than in healthy subjects of the same age. "The phenotype of their T cells appeared older than those of people without the chronic inflammatory process," she told Agência FAPESP. The study was part of her Ph.D. research at FM-USP.
The results for the group of smokers suggested that moderate to intense smoking did not accelerate immunosenescence when compared with the results for healthy adults. "COPD affected the patients more than aging, drastically impairing the immune system," said Thalyta Nery Carvalho Pinto, a Ph.D. candidate and second author of the article.
In her 2016 master's dissertation, Fernandes studied the effects of physical exercise on the immune response of COPD patients, showing that rehabilitation slowed cellular senescence on some parameters and boosted the contribution of T cells to the immune response. The results suggested that COPD patients had a higher proportion of exhausted T cells as well as diminished functional capacity. "Our recent study set out to see what cell types are involved in COPD and aging," she said.
Three stages
Immunosenescence is defined as a decline in the immune system function during aging. It affects both innate and adaptive immunity. It is characterized by a decrease in "naive" T cells, which have matured but have not yet been activated by encountering their antigens, and an increase in "memory" (antigen-experienced) T cells.
Memory T cells undergo three stages of development during a person's lifetime. In the first, which lasts until about age 10, a pool of naive cells becomes memory cells in response to stimulation by specific antigens. In the second (known as memory homeostasis), circulating memory T cells reach a plateau and remain there until adulthood. In the third, the frequency and functionality of these cells change after a long period of stability, leading to an increase in susceptibility to infections caused by immune dysregulation as part of the person's aging and physiological decline.
In the study, the researchers found that this stage of immune system development was disrupted in COPD patients, who exhibited a reduced pool of naive cells available to respond to pathogens, and (paradoxically) a larger proportion of these cells impaired by late differentiation, senescence or exhaustion than healthy older adults and smokers.
"We also found that immunosenescence and the alterations seen in COPD patients were most pronounced in CD8+ T cells, which can be considered 'soldiers' that carry out the immune system's orders by killing invaders," Benard said.
The same researchers are now studying, in a different group of volunteers, how B cells (the immune cells that produce antibodies) respond in COPD patients, and how these patients are responding to COVID-19 vaccines.
More information: Juliana Ruiz Fernandes et al, Age-associated phenotypic imbalance in TCD4 and TCD8 cell subsets: comparison between healthy aged, smokers, COPD patients and young adults, Immunity & Ageing (2022). DOI: 10.1186/s12979-022-00267-y