Direct breastfeeding feasible for NICU babies with new standardized approach
A new standardized approach to feeding premature infants in the hospital, dubbed the Encourage, Assess, Transition (EAT) protocol, increases the prevalence of direct breastfeeding without increasing the length of time the infant is hospitalized. That conclusion from a quality improvement project by Nellie Munn Swanson, DNP, MPH, APRN, CPNP-PC, CLC, of the University of Minnesota School of Nursing, and colleagues is reported in Advances in Neonatal Care.
"Direct breastfeeding is often an exception, rather than standard care for preterm infants hospitalized in the U.S.," Dr. Swanson and her colleagues explain. Yet from the parent perspective, "direct breastfeeding has deep meaning beyond nutritional value," the authors say, especially for building a bond with the baby. The term direct breastfeeding is defined as feeding the infant directly from the breast, whereas breastfeeding can also include providing expressed mother's milk with a bottle.
At the hospital where the quality improvement project was implemented, many parents of preterm infants reported they did not receive adequate assistance to meet their direct breastfeeding goals. In response, Dr. Swanson and a team of colleagues conducted a literature search and found strong evidence for practice change, including the Spatz 10-step model for human milk and breastfeeding, an evidence-based intervention designed to support human milk feeding and breastfeeding for hospitalized newborns.
New model for breastfeeding in the NICU
Dr. Swanson adapted this model to improve hospital practices specific to direct breastfeeding using a nurse-led protocol that has three phases:
- Encourage—The mother/lactating parent begins pumping milk within 1 hour of birth if possible; the baby begins tube feeding but also receives drops of the mother's milk for taste; mother and baby have skin-to-skin contact; the mother practices feeding the baby on a dry breast
- Assess—The baby is evaluated regularly to see whether it is ready for coordinated sucking, swallowing, and breathing, and parents are given advance notice of oral feeding readiness
- Transition—The baby has at its first feed at the breast; direct breastfeeding is alternated with tube feeding; bottle feeding is avoided; the baby is weighed regularly to determine whether it's getting enough milk (conventionally, this decision is based on the number of minutes the baby is latched at the breast)
All elements of the EAT protocol were already being applied in Dr. Swanson's hospital, as they are in other healthcare systems. However, they were used inconsistently, depending on the preferences of individual healthcare professionals. The value that Dr. Swanson's team added was to create a standardized, step-by-step approach and train healthcare professionals to carry it out. The team also created educational materials for parents to help them advocate for their goal of direct breastfeeding.
Powerful pilot results
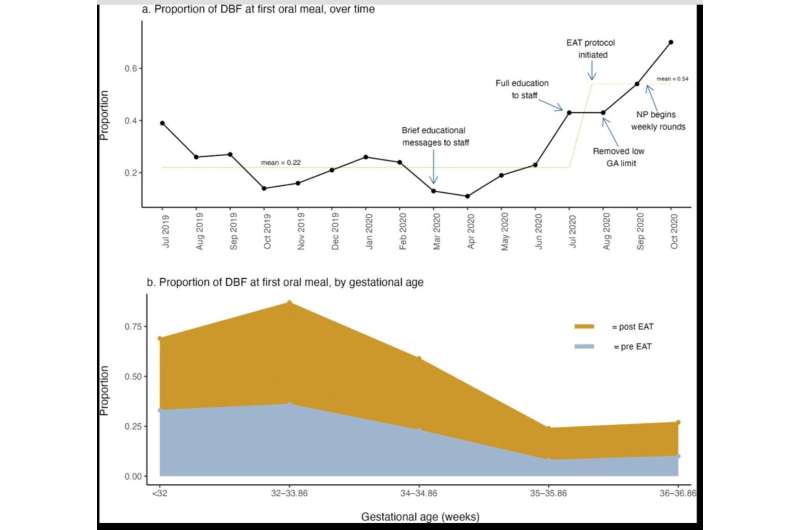
Dr. Swanson's team ran a pilot of the EAT protocol from July to October 2020. The 85 preterm infants seen during that period were compared with 364 preterm infants hospitalized between July 2019 and July 2020, before the protocol was launched. Both groups included all infants whose parents planned for feeding with mother's milk, not just those whose parents planned to directly breastfeed. The main measures were:
- Direct breastfeeding at first oral meal—22% of infants before protocol launch and 54% after, a 145% increase
- Average number of direct breastfeeding meals during an infant's hospital stay—13 before protocol launch and 20 after, a 53% increase
- Average number of times babies were weighed—110 per month before protocol launch and 293 after, an increase of 166%
- Length of infant's hospital stay—Similar in the two time periods
The pilot "provides further evidence that the method of first oral feeding influences direct breastfeeding outcomes in hospitalized preterm infants," the authors conclude. "For parents with a goal to directly breastfeed their infant, it is critical that clinicians prioritize direct breastfeeding, and provide both educational and tangible assistance for direct breastfeeding in the hospital."
More information: Nellie Munn Swanson et al, Encourage, Assess, Transition (EAT), Advances in Neonatal Care (2022). DOI: 10.1097/ANC.0000000000001037

















