This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Normal result from gastrointestinal biopsy not protective against later IBD, study finds

Individuals with a gastrointestinal (GI) biopsy that comes back normal still have a heightened risk of inflammatory bowel disease (IBD) in the years following that normal biopsy than their population references, according to a new study publishing February 23 in the open access journal PLOS Medicine by Dr. Jiangwei Sun of Karolinska Institutet, Sweden, and colleagues.
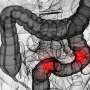
IBD is a chronic disease of the GI tract and subtypes mainly include Crohn's disease and ulcerative colitis. The disease is typically diagnosed with an upper or lower GI biopsy, taken during an endoscopy. In clinical practice, the most frequent finding on an endoscopy is a normal biopsy, and evidence suggests a persistently decreased risk of colorectal cancer for up to ten years after a normal biopsy. However, the association between a normal biopsy and a later diagnosis of IBD has been unclear; some studies have hinted that IBD may have a symptomatic period before diagnosis is possible.
In the new study, researchers used a Sweden-wide database of GI biopsy reports from 1965 to 2016 to identify 200,495 individuals with a normal lower GI biopsy and 257,192 individuals with a normal upper GI biopsy. They also identified more than 2 million matched population references from the Swedish Total Population Register, and nearly half a million siblings of the biopsied individuals who were alive and had not had their own GI biopsy from the Swedish Multi-Generation Register.
During a median follow up time of 10 years, 4,853 individuals (2.4%) with a normal lower GI biopsy developed IBD, compared to 0.4% of the population references. This translated to one additional IBD case for every 37 individuals during the 30 years after a normal lower GI biopsy.
The individuals with normal lower GI biopsy had a higher risk of overall IBD (HR=5.56; 95%CI: 5.28–5.85), ulcerative colitis (HR=5.20; 95%CI: 4.85–5.59) and Crohn's disease (HR=6.99; 95%CI: 81 6.38–7.66) than the population references. The risks were 3.27 (95%CI: 3.05–3.51) for overall IBD, 3.27 (95%CI: 2.96–3.61) for ulcerative colitis, and 3.77 (95%CI: 3.34–4.26) for Crohn's disease than their siblings.
A normal upper GI biopsy was also associated with an increased risk of Crohn's disease compared to both the population references and siblings (HR=2.93; 95%CI: 2.68–3.21 and HR= 2.39; 95%CI: 2.10–2.73). The study was limited by a lack of data on the indications for each patient's biopsy, patients' lifestyle, medical background, and genetics.
"Endoscopic biopsy with normal mucosa was associated with an elevated IBD incidence for at least 30 years. This may suggest a substantial symptomatic period of IBD and incomplete diagnostic examinations in patients with early IBD," the authors say. "Clinicians should be aware of the long-term increased risk of IBD in those with symptoms requiring GI investigation but with a finding of histologically normal mucosa."
More information: Long-term risk of inflammatory bowel disease after endoscopic biopsy with normal mucosa: A population-based, sibling-controlled cohort study in Sweden, PLoS Medicine (2023). DOI: 10.1371/journal.pmed.1004185