This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
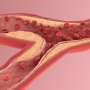
Biodegradable polymer system offers new hope for treating rheumatoid arthritis

A team led by engineers at the University of California San Diego has developed a biodegradable polymer system to treat rheumatoid arthritis, an autoimmune and inflammatory disease, by working in concert with the power of the human immune system.
The research builds on increasing clinical interest in modulating the immune system to treat cancers and autoimmune disease, as well as previous work with all-trans retinoic acid (ATRA) which is produced naturally in the body and helps cells grow and develop. By approaching these challenges from the perspective of a biomaterials engineering lab, the team adds two key innovations to previous methods: local release and harnessing the joint microenvironment for sustained effectiveness.
With this method, encapsulated ATRA is injected directly into a joint affected by rheumatoid arthritis, where it remains in effect for at least several weeks. During that time, ATRA transforms disease-causing cells into disease-stopping cells, known as regulatory T cells, which can treat or prevent the disease elsewhere in the body.
"Essentially, our system turns the disease site into a factory that produces regulatory T cells," said David A. McBride, a chemical engineering graduate student at UC San Diego supervised by nanoengineering professor Nisarg Shah. "It uses a biodegradable biomaterial to facilitate the timed release of ATRA, which reprograms T cells so they can treat disease."
The research was published in Advanced Science. McBride is a co-author on the paper.
"This is a very promising line of research utilizing the latest and greatest technology in immunoengineering to combat arthritis," said Iannis Adamopoulous, an associate professor of medicine at Harvard's Beth Israel Deaconess Medical Center, Department of Medicine, Division of Rheumatology.
What is ATRA?
ATRA is a small molecule currently FDA approved to treat acute promyelocytic leukemia (APML). Research over the last two decades has suggested that it also has promise in treating autoimmune arthritis and relieving inflammation. However, that method relies on ATRA traveling freely throughout the body, which can cause immunosuppression and potentially significant off-target toxicity, along with other unwanted side effects.
"Previous work established that ATRA has potential in treating autoimmune arthritis, but the route of administration precluded the work from being relevant to clinical translation," said McBride.
When ATRA is encapsulated using biodegradable materials, it can be injected directly into joints at therapeutic concentrations but as it diffuses out of the joint, it enters circulation at much lower concentrations, minimizing or preventing unwanted effects. Without the controlled release afforded by the biomaterial encapsulation, patients would require multiple injections per day to achieve the same effects, which would be impractical in most cases.
How it works
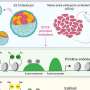
When the human immune system functions properly, helper T cells patrol the body in search of disease-causing pathogens. When a pathogen is detected, a helper T cell can recruit additional cells to help fight it. "It's kind of similar to how you might have police cars roaming the city, and when one sees a crime occurring, they call for backup to get the situation under control," said McBride.
Many autoimmune diseases result from cases of "mistaken identity," in which these cells attack a perceived danger target that is in fact a part of normally functioning cells in the body. The subsequent proliferation of such pathogenic T cells, which McBride calls "bad apples," can result from a combination of genetic and environmental factors and wreak havoc on the body when they summon large teams of immune cells for unnecessary standoffs.
For example, "in type 1 diabetes, you have bad apples that call in reinforcements against your pancreas," said McBride. "In multiple sclerosis, it is against your neurons. In rheumatoid arthritis, it is against your joints. So, your immune system recognizes this as something to be attacked, and it goes and recruits a bunch of additional immune cells to these places and fights a war until all the pathogens are gone. Except that, in this case, it's not attacking pathogens, but healthy parts of the body."
Many current approaches block the chemical signals that immune cells use to communicate, effectively preventing the pathogenic T cells from calling in reinforcements without eliminating the "bad apples." Time-released ATRA reprograms them to act as regulatory T cells, or "good apples." These cells still have the ability to recognize and activate in the joints, but rather than calling in additional immune cells, they help to resolve the inflammation. In areas such as joints, which aren't recommended for repeated injections, the sustained-release formulation allows sufficient therapeutic exposure to flip the balance.
ATRA makes lasting modifications to the ability of cellular machinery to read cell DNA, improving the function of the anti-inflammatory regulatory T cells. This treats T cells at the site of disease and generates regulatory T cells specific to that diseased tissue. Then, when these cells move to other disease locations, they can help resolve inflammation and promote healing. Because the cells are specific to the disease, they don't interfere with normal immune function, allowing them to supplement existing therapies or provide alternatives for patients who need them.
"The coolest part about this is that the treated site of disease, where the bad apples were previously proliferating, now becomes a place that can generate regulators that can now go patrol the body and actually prevent disease," said McBride.

The limitations of existing approaches
Patients with rheumatoid arthritis are frequently treated with disease-modifying anti-rheumatic drugs (DMARDs) and in many patients this approach works well. However, about a third of patients don't adequately respond to front-line DMARDs, and they come with some significant disadvantages.
First, while using DMARDs, some patients become more susceptible to infectious disease and exhibit weaker responses to vaccines. In this regard, "the COVID-19 pandemic has brought a lot more understanding on the risks of immunosuppression into public awareness," said McBride.
Additionally, because most immunosuppressives currently used to treat rheumatoid arthritis stay in the system for up to two weeks, there is no option to discontinue treatment if a dangerous infection occurs. This is compounded when patients use two or more treatments simultaneously, which is not uncommon due to the complexity of the disease. Using multiple powerful immunosuppressants can exacerbate the risks of infections or cancer.
"If you can instead have a treatment option that doesn't have an immunosuppressive effect, you can really reduce the risk for patients that need multiple treatment modalities to keep their autoimmune disease in check," McBride said.
Finally, for some patients, immunosuppressives work well for a time and then lose their effectiveness. This can happen when their bodies develop antibodies that neutralize the medications or new disease pathways emerge. New treatments like this one could potentially supplement DMARDs, compensating for waning effectiveness or requiring lower doses to start with.
"In well controlled patients, reducing or eliminating the need for immunosuppressive drugs is desirable," said Shah. "However, when it is attempted, studies have shown that the disease can flare up again. So having a non-immunosuppressive option could go a long way."
Research methods, challenges and next steps
The team tested its biomaterial-encapsulation method using a combination of mouse and human cells. After this achieved positive results, they transitioned to mouse models of autoimmune arthritis, coming closer to simulating the remarkable complexity of a real-life case of autoimmune disease in a human subject.
The work required multiple models of disease, each designed to demonstrate a specific aspect of the team's hypothesis, as well as rigorously tracking the cells from their origin points at injection to the other locations where they recirculated and proved effective in fighting disease.
Currently, the researchers are actively working toward commercialization. "As this is my first experience with something like this, it is difficult for me to estimate, but we are currently targeting approval to start clinical trials within five years," said McBride. To evaluate possible commercialization routes, McBride has participated in the UC San Diego Institute for the Global Entrepreneur (IGE) NSF I-Corps and MedTech Accelerator programs.
More information: David A. McBride et al, Immunomodulatory Microparticles Epigenetically Modulate T Cells and Systemically Ameliorate Autoimmune Arthritis, Advanced Science (2023). DOI: 10.1002/advs.202202720