This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
Why new cancer treatment discoveries are proliferating
In the five years since the FDA's initial approval of chimeric antigen receptor (CAR) T cell therapy, Penn Medicine has gleaned 20 additional approvals related to drugs and techniques to treat or detect cancer.
Rather than being the single disease class many people refer to, "cancer" is a blanket term that covers more than 100 distinct diseases, many of which have little in common aside from originating with rapidly dividing cells. Since different cancers demand different treatments, it follows that any given new therapy emerging from any institution would be likely to be a new cancer treatment.
But why so many in just this five-year period?
The volume of new cancer treatments makes sense, says Abramson Cancer Center (ACC) Director Robert Vonderheide, MD, DPhil, attributing the flurry of new cancer drug approvals to a recent "explosion" in knowledge about cancer biology.
"Much of that knowledge is about the immune system's ability to attack cancer, which people seriously doubted until about 20 years ago. As soon as we had a clinical validation for this Achilles heel in cancer, the dam burst for ideas about other ways to exploit that vulnerability to come forward," he says. "The first drug that came out to activate the immune system inspired the rest of the field to find the next drug, and the one after that. We as a field have moved from serendipity and empiricism to science-driven drug design."
The first CAR T cell therapy approval invigorated Penn faculty interested in finding new ways to harness the immune system to fight cancer.
"An approval like that makes what you're working on more of a reality," says Avery Posey, Ph.D., an assistant professor of Systems Pharmacology and Translational Therapeutics in the Perelman School of Medicine, whose lab team spends much of its time trying to identify more specific antigens for solid tumors and also studies ways to optimize engineered donor T cells. "It brings a new perspective, showing that your work is more than basic research and can actually become drugs that impact patients' lives. That's a real motivator to keep pushing forward."
For cancer, new treatments are not just immunotherapies
Honing new immunotherapies is a priority among Penn researchers, but not every recently approved new cancer treatment or detection tool developed at the institution engages the immune system. Faculty have explored and introduced widely varying approaches to improving the standard of care for cancer patients.
For example, there's olaparib (marketed as Lynparza), which is used in ovarian cancer and breast cancer, most commonly tumors involving an inherited BRCA gene mutation. The oral medication works by targeting PARP, an enzyme in the body that helps to repair damaged cells—including cancer cells. By inhibiting PARP, the drug stops the repair of cancerous cells to prevent them from growing. The drug's approvals in 2014, 2018 and 2022 were based on clinical trials led or co-led by Susan Domchek, MD, executive director of the Basser Center for BRCA at the ACC.
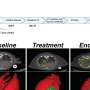
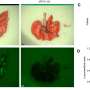
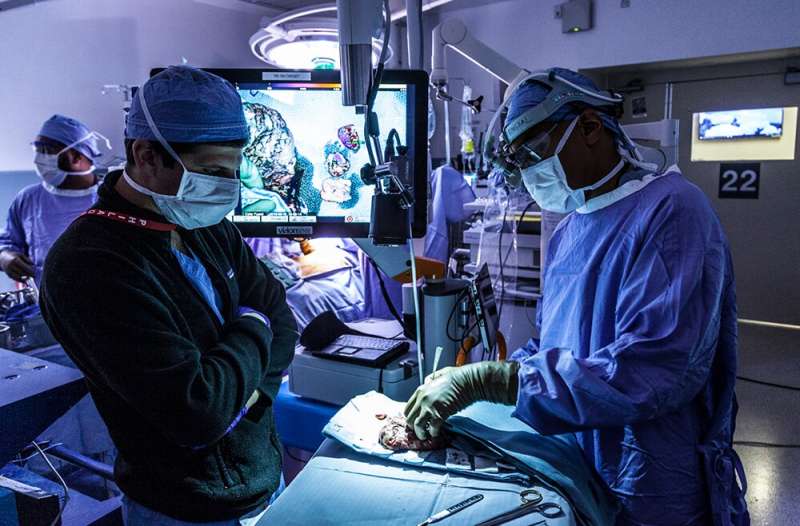
There's also pafolacianine (marketed as Cytalux), the first FDA-approved agent that illuminates ovarian cancer and lung cancer lesions during surgery, enabling surgeons to find and remove cancerous tissue. Penn investigators Janos Tanyi, MD, Ph.D., and Sunil Singhal, MD, led its Phase 2 and 3 clinical trials leading to approval. And belzutifan (marketed as Welirig), the first treatment of its kind to treat or intercept cancer in von Hippel-Lindau disease-associated tumors, such as those in renal cell carcinoma and central nervous system hemangioblastomas—a new cancer drug with Penn connections from basic science discovery about cancer hypoxia through to the definitive clinical trial leading to its approval.
Cancer patients survive longer, offering hope for other diseases
On Jan. 12, 2023, the American Cancer Society released its annual compilation of cancer facts and trends, which reported that since its peak in 1991, cancer mortality in the U.S. has dropped 33%.
"That's almost 4 million deaths averted. Clearly, something dramatic has changed the outlook for patients with cancer in this country in the last 30 years," Vonderheide says. "Much of that has to do with new therapies, which were all unknown drugs in a phase one clinical trial at some point. Every single drug you see advertised on TV—once upon a time, some patient somewhere was the first patient ever treated with it. This is why we do what we do."
Because of high mortality outcomes among cancer patients who haven't responded to conventional therapies, risk tolerance in cancer clinical trials tends to be higher than in trials testing novel therapies for non-cancer conditions, explains Emma Meagher, MD, senior vice dean for clinical and translational research in the Perelman School of Medicine.
"High-risk, and potentially high-reward, trials happen frequently in cancer for that reason and oftentimes can move more quickly," Meagher says.
Just because a new drug is first tested and approved to treat cancer doesn't mean it can only treat cancer, though. Many therapies that start in oncology eventually have broader disease applications—like CAR T cell therapy, which is already showing promise with other diagnoses, like the autoimmune disease lupus.
CAR T cell therapy's potential translation to other diseases is "a rumble that is beginning to sound like thunder in autoimmune disorders, neurological conditions, rheumatological conditions, and dermatological conditions, among others where immune mechanisms are implicated," she adds. "We're beginning to see momentum in using what is currently considered a cancer therapy well outside of the oncology space, and I predict that Penn will be a real leader in this area."