This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
Brain waves may predict cognitive impairment in Parkinson's disease
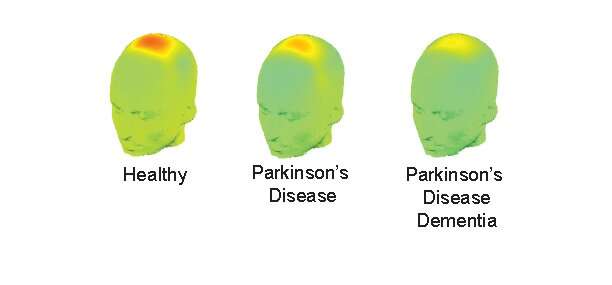
A few minutes of data recorded from a single electrode placed on top of the head may be sufficient to predict thinking problems, including dementia, in patients with Parkinson's disease (PD). The finding from a new University of Iowa study might help improve diagnosis of cognitive disability in PD and develop new biomarkers and targeted therapies for cognitive symptoms of the disease.
"Cognitive decline, including dementia, is a significant and underappreciated symptom of Parkinson's disease. Around 30% of patients can have cognitive symptoms at the beginning of the disease, and up to 80% will have cognitive problems at some point in their disease," says Nandakumar Narayanan, MD, Ph.D., associate professor of neurology at the UI Carver College of Medicine and senior author of the new study, which is published in the Journal of Neurology, Neurosurgery & Psychiatry. "Furthermore, although we have quite a few effective treatments for the motor symptoms of Parkinson's, including medical therapies and deep brain stimulation, we have very few treatments for the cognitive aspects of Parkinson's disease."
EEG: A potential tool for predicting cognitive function in Parkinson's
The brain recordings were made using a very old, widely available technology called electroencephalography (EEG), which measured low-frequency brain waves, known as delta and theta waves, in the frontal region of study participants' brains. The UI team found that reduced strength of these specific brain waves when a patient is required to engage in thinking is strongly linked to cognitive dysfunction in PD. The findings suggest that EEG, which is also inexpensive and non-invasive, might be useful for diagnosing cognitive impairment in PD patients.
"Traditional methods for diagnosing cognitive problems often involve time-consuming pen and paper tests and require a neurologist to administer and interpret the tests. In addition, because these traditional tests can be 'learned," they cannot be used repeatedly over time for the same patient," says Narayanan, who also is a neurologist with UI Health Care and a member of the Iowa Neuroscience Institute. "In contrast, EEG can be done continuously over several hours or days. It can be applied in nursing homes, or patient's homes, and it gives you a richly featured description of a patient's cognitive status."
The EEG measurements might also be useful for monitoring and fine tuning the cognitive side effects of medications and brain simulation used to treat for Parkinson's disease. Eventually, EEG could even provide a basic assay to determine whether new treatments for PD are effective at improving cognitive function.
Diminished brain signal linked to cognitive problems in Parkinson's
Lastly, the study, which is one of the largest to date, involving 100 PD patients across the full spectrum of cognitive function from healthy to dementia, and 49 demographically similar control participants, reveals a fundamental insight into the role of the brain signal being measured by the EEG electrode.
All the participants completed three different tasks that are commonly used to assess cognitive control, and while they were doing the tasks, a single EEG electrode measured the strength of the low frequency delta and theta brain waves from their frontal cortex.
Narayanan's team found that diminished cognitive function was correlated with diminished strength of low frequency brain waves while the patient was doing a task. Importantly, it did not matter which cognitive task the patient was doing during the measurement.
"Surprisingly, the effect was seen simply because the patient was required to pay attention to a cue and respond. I think this is the deep insight into why Parkinson's patients have cognitive problems: They fail to engage these basic response processes in the brain," Narayanan explains.
"That was very surprising to us, and it's helpful because it means we might be able to get information about cognitive function using the simplest version of this task where there's a cue, and the patient has to engage and respond. That process—cue, engage, respond—might be enough to determine where patients are on the cognitive status scale and whether they have the potential to improve."
Narayanan says this insight might also be an opportunity to help patients. Potentially "cueing" Parkinson's patients to engage in a task—whether it's walking, talking or thinking, might improve how well they perform the task. If this is true, it would have important implications for the way rehabilitation, occupational, and speech therapists help patients with PD.
The next steps for Narayanan's team are to investigate the mechanisms that link diminished delta and theta brain waves to worse cognition in PD, and to better understand how EEG technology might be used to improve diagnosis or even treatment of cognitive dysfunction in patients with PD.
In addition to Narayanan, the research team included Arun Singh, Ph.D., at University of South Dakota; Rachel Cole, Arturo Espinoza, and Jan Wessel at the UI; and James Cavanagh at the University of New Mexico.
More information: Arun Singh et al, Evoked mid-frontal activity predicts cognitive dysfunction in Parkinson's disease, Journal of Neurology, Neurosurgery & Psychiatry (2023). DOI: 10.1136/jnnp-2022-330154