This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
proofread
Researchers uncover molecular pathways underlying depression
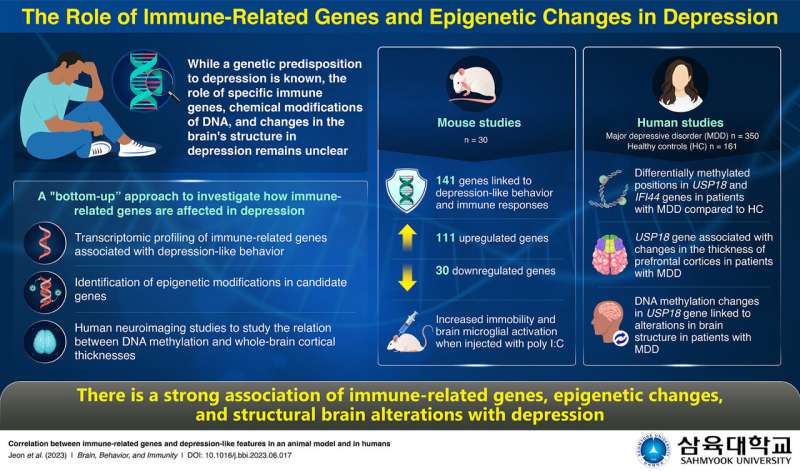
Depression is a common mental health problem that affects people across demographics. Scientists have long known that there may be a genetic component that confers predisposition to depression, but the specific underlying mechanisms have remained elusive. Growing evidence indicates that inflammation and immune-related processes in the brain could play a significant role in depression.
A team of researchers including Dr. Se Jin Jeon from Sahmyook University conducted a study to gain deeper insights into these mechanisms. Their study was published in Brain, Behavior, and Immunity.
The team employed a mouse model to measure their immobility, a behavior linked to depression, using a forced swim test. Through transcriptional profiling, they found that 141 genes significantly correlated with immobility, with 111 upregulated and 30 downregulated.
"We found that these genes were related to the interferon pathway, which is involved in the regulation of inflammation in the body," explains Dr. Jeon. The researchers further validated their findings through real-time PCR, confirming that immune-related genes were expressed at higher levels in mice with higher immobility scores.
Additionally, they induced immune responses using an intracerebroventricular injection, which resulted in increased immobility and microglial activation, providing further evidence regarding the link between immune response genes and indicators of depression.
Leveraging the findings of murine study, the team aimed to understand the link between DNA methylation, brain structural changes, and depression in humans. For this, 350 patients with major depressive disorder (MDD) and 161 healthy controls were examined. DNA methylation analysis—a technique used to study the epigenetic modifications on DNA—was conducted on the genes USP18 and IFI44, since these were found to be associated with depression-like behavior in mice and were involved in interferon signaling pathways.
The researchers found differences in methylation patterns between patients with MDD and controls. In patients with MDD, DNA methylation of a specific region in the USP18 gene correlated with reduced thickness in several brain regions associated with emotions and cognition. Meanwhile, in the control group, DNA methylation of another region in USP18 correlated with increased thickness in brain regions linked to vision and sensory processing.
These findings link not only the expression of immune-related genes, but also their epigenetic status and their effect on brain structure, with depression.
"In summary, we found elevated expression of inflammation-related genes in patients with depression compared to controls. This can increase inflammatory conditions in the body, including the brain, and ultimately lead to structural abnormalities in brain regions involved in emotional regulation, which may contribute to the development of depression," concludes Dr. Jeon.
Thus, with the potential to serve as viable treatment targets, these immune genes offer an alternative approach or supplement to the currently approved pharmacologic treatments.
More information: Edson Luck Gonzales et al, Correlation between immune-related genes and depression-like features in an animal model and in humans, Brain, Behavior, and Immunity (2023). DOI: 10.1016/j.bbi.2023.06.017