This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
New way to kill breast cancer stem cells that have ancestral features and resist chemotherapy
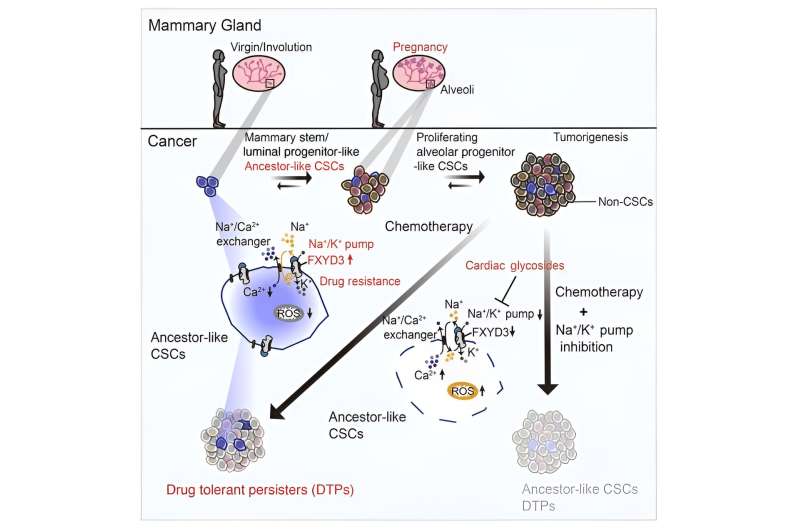
Researchers at Karolinska Institutet and Kanazawa University in Japan have made a new discovery that could improve breast cancer treatments. The researchers studied cancer stem cells (CSCs), which can resist chemotherapy and form new tumors. They found a type of CSC that is vulnerable to drugs that target a pump in the cells. These drugs could potentially kill these CSCs and help patients with triple-negative breast cancer (TNBC), a hard-to-treat form of breast cancer.
The work is published in the Journal of Clinical Investigation.
Breast cancer is a complex and diverse disease that affects millions of women worldwide. One of the challenges in treating breast cancer is that some of the cancer cells have the ability to survive chemotherapy and form new tumors. These cells are called cancer stem cells (CSCs), and they are not all the same. Some CSCs have different features and behaviors than others, which makes them harder to target.
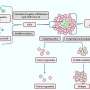
"We used a technique called single-cell RNA sequencing to analyze the diversity of CSCs in a type of breast cancer called triple-negative breast cancer," says Associate Professor Theodoros Foukakis at the Department of Oncology-Pathology. TNBC is an aggressive and hard-to-treat form of breast cancer that does not respond to hormone therapy or targeted drugs.
The researchers found that there is a subpopulation of CSCs that has ancestral features, meaning that they resemble the cells that form the breast tissue during pregnancy. These CSCs are marked by a protein called FXYD3, which is part of a pump that regulates the balance of sodium and potassium ions in the cells. Interestingly, following chemotherapy, these cells persisted in resistant tumors but diminished in responding tumors.
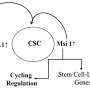
The researchers discovered that FXYD3+ CSCs are more likely to evolve and proliferate, and that they have traits of alveolar progenitors, which are cells that form the milk-producing glands in the breast. These cells are normally induced during pregnancy, but in TNBC they can contribute to tumor growth and spread.
The researchers also found that FXYD3+ CSCs are more resistant to chemotherapy, and that they persist after treatment, making them potential sources of tumor recurrence. They identified FXYD3+ CSCs as crucial therapeutic targets, and suggested that eliminating them could improve the prognosis of TNBC patients.
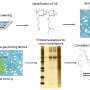
To test this idea, the researchers used drugs that inhibit the sodium–potassium pump, such as cardiac glycosides, which are normally used to treat heart failure. They found that these drugs were effective in killing FXYD3+ CSCs, both in the laboratory and in animal models. They also found that these drugs could enhance the effect of chemotherapy, and prevent the formation of new tumors from FXYD3+ CSCs.
In summary, the researchers have uncovered a paradoxical role of FXYD3+ CSCs in TNBC. These CSCs have ancestral features that make them more adaptable and aggressive, but also more vulnerable to drugs that target the sodium–potassium pump. By exploiting this weakness, the researchers have proposed a new strategy to eliminate CSCs that are drivers of tumor plasticity and chemoresistance in TNBC. This could lead to better outcomes for patients with this challenging disease.
More information: Mengjiao Li et al, FXYD3 functionally demarcates an ancestral breast cancer stem cell subpopulation with features of drug-tolerant persisters, Journal of Clinical Investigation (2023). DOI: 10.1172/JCI166666