This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Scientists analyze antibody responses to SARS-CoV-1 and SARS-CoV-2 infections
After the outbreak of the novel coronavirus in 2020, vaccines, antibodies (Abs), small molecule drugs, and other interventions needed to be researched, and such a rapid development is partly due to the accumulation of scientific research on severe acute respiratory syndrome virus (SARS virus, SARS-CoV-1), MERS-CoV, and other coronaviruses that cause human disease.
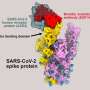
SARS-CoV-1 and SARS-CoV-2 are members of the beta coronavirus and share similarities in the structure and function of the surface membrane protein Spike, and both enter cells through the interaction between the viral spike (S) glycoprotein and the angiotensin-converting enzyme 2 (ACE2) receptor on the host cell surface. However, due to the limitations of technology and methodology, there exist many questions in the characteristics of SARS-CoV-1 antibody response and the relationship with to SARS-CoV-2 antibody response.
Researchers led by Prof. Yang Yuhe from the National Center for Nanoscience and Technology of the Chinese Academy of Sciences, Prof. Zhang Linqi from Tsinghua University, and Prof. Li Taisheng from Peking Union Medical College Hospital have analyzed the antibody response of SARS-CoV-1 convalescents from the aspects of polyclonal antibodies (pAbs) and monoclonal antibodies (mAbs), and they compared the duration, classification and properties of receptor-binding domain (RBD) Abs.
The results were published in Immunity.
Using blood samples from SARS convalescents during their recovery period that had been stored for 20 years, the researchers systematically analyzed the antibody responses of SARS-CoV-1 patients, and made a comprehensive comparison with the antibody responses of SARS-CoV-2 patients.
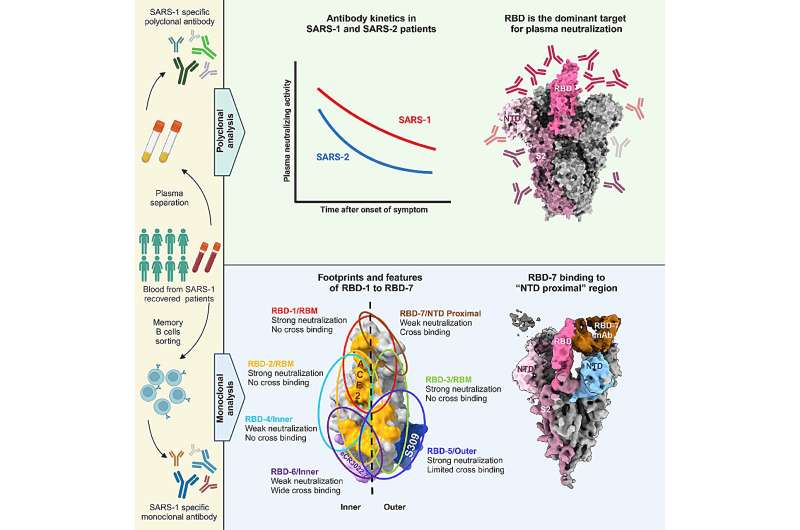
According to the researchers, the plasma neutralization titer of SARS-CoV-1 convalescents was higher than that of SARS-CoV-2 severe convalescents, and the duration was longer. One reason may be the higher proportion of antibodies targeting SARS-CoV-1 RBD. In addition, cross-binding of plasma from SARS-CoV-1 convalescents is high, but the cross-neutralization is low, suggesting differences in spike gene sequence, protein structure, and immunogenicity between the two viruses.
They isolated 77 mAbs from SARS-CoV-1 convalescents, 60 of which targeted the RBD and most of which showed strong neutralization with SARS-CoV-1, while the other 17 non-RBD Abs showed little or no neutralization. In addition, the neutralization proportion of these RBD Abs was significantly higher than that isolated from SARS-CoV-2 convalescents, consistent with the result of the plasma antibodies response.
The antibodies induced by two coronaviruses have a similar high frequency of mutation after infection, indicating that the mutation and maturation rate of antibody genes follow the internal rhythm of the human body and are independent of the type of virus or the infection severity.
They then analyzed the structure and function of 60 RBD-targeting antibodies. These 60 RBD-targeting antibodies were classified into seven groups by competitive SPR analysis with ACE2 or typical antibodies with known epitopes, named RBD-1 to 7. RBD 1-3 are RBM antibodies that strongly compete with ACE2 and 80R, and have different competitiveness with S230, m396 and S309, respectively.
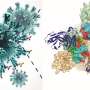
Subsequently, the binding modes and specificities of 21 selected Abs from the seven groups to the spike of SARS-CoV-1 were further characterized by single-particle, negative-stain electron microscope (ns-EM).
RBD-1 Abs bound to the "peak" of the RBD, RBD-2 Abs bound to the "mesa" and inner ridge of the RBM, RBD-3 Abs targeted to the outer ridge of RBM, RBD 1-3 Abs showed high neutralization to SARS-CoV-1 and weak cross activity. However, RDB-5 and RDB-6 Abs do not compete strongly with ACE2, and the binding sites mainly include the outer face (RDB-5) or the inner face (RDB-6) of RBD.
RBD-6 Abs has weak neutralization but strong cross-reactivity, the IgG and Spike trimer complexes all form the dimers-of-trimers or trimers-of-trimers conformation.
RBD-7 Abs target a specific region on the "up" RBD that interfaced with the N-terminal domain (NTD) of the adjacent spike protomer (NTD proximal). Abs targeting this epitope are extremely rare in reported human COVID-19 convalescents, but account for a large proportion (13/60) of SARS-CoV-1 convalescents and share the same V region gene, which is one of the characteristics of antibody response in SARS-CoV-1 convalescents.
Finally, the team evaluated the cross-neutralization of eight Abs against several novel coronavirus mutants and other ACE2 receptor coronaviruses, and analyzed the structure of the spike protein complex of two cross-antibodies (W328-6A1 and W328-6E10) by cryo-electron microscopy (cryo-EM). It provides structural information for further understanding of the broad neutralization mechanism.
"This work explores the SARS-CoV-1 antibody field, and in parallel explores the antibody response to COVID-19, so we believe that this research perspective will be very valuable. The antibody response caused by SARS-CoV-1 and SARS-CoV-2 infection has many similarities, such as their antibodies can cross each other, and the RBD antibodies mainly contribute to the neutralization," said Prof. Zhang Linqi.
"This study firstly classifies RBD-targeting antibodies of SARS, provides important basis and guidance for the development of new-generation broad coronavirus antibody drugs and vaccines," said Prof. Yang Yuhe.
More information: Ruoke Wang et al, Dissecting the intricacies of human antibody responses to SARS-CoV-1 and SARS-CoV-2 infection, Immunity (2023). DOI: 10.1016/j.immuni.2023.10.007