This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
written by researcher(s)
proofread
Affordable stroke-risk screening could save the lives of many children with sickle cell disease in sub-Saharan Africa

Most of the estimated 300,000 babies born every year with sickle cell disease, an inherited red blood cell disorder, live in sub-Saharan Africa in nations where there are few resources to treat them.
As an assistant professor of biomedical engineering, I am working to reduce the likelihood that children born with sickle cell disease will die from stroke, one of the most common complications.
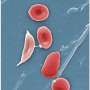
Sickle cell disease, whose name reflects the disease's sickle or crescent moon shape of red blood cells, can affect any major organ, but my primary concern is its effect on the brain. It causes a lower oxygen level and abnormal blood flow in the brain, which is associated with a high risk of stroke. Without treatment, 11% of children with sickle cell disease will have a stroke before they turn 20 years old.
The mortality rate for children younger than 5 years old is 50% to 80%. The majority of sickle cell patients share an African heritage. The places where malaria rates were high historically have the highest sickle gene frequency because it provides protection against the mosquito-borne disease.
Fewer resources for screening
In an advanced nation like the U.S., children are more likely to receive stroke-risk screening and start a regular blood transfusion therapy if the need is there.
In sub-Saharan African nations, there are few resources for screening. The current screening tests use an ultrasound system called a transcranial Doppler to identify elevated blood flow to the brain. But they aren't affordable, and only a few hospitals in sub–Saharan Africa have certified operators.
My goal, thanks to a US$426,000 grant from the National Institutes of Health for a three-year study, is to develop a low-cost, light-based device that can noninvasively measure brain blood flow in children with sickle cell disease and determine an affected child's risk of stroke. The plan is then to disseminate this device to southern African countries, increasing the number of children who get access to the screening protocol.
Saving families the anguish
Not only would a low-cost testing solution allow an underserved community's needs to be addressed, but it would save countless families the anguish that comes with a diagnosis.
Patients have a chronic shortage of healthy red blood cells, are more susceptible to clots when their abnormal sickle-shaped blood cells pass through small blood vessels, and experience tremendous pain from that. In fact, pain is the top reason that sickle cell patients go to the emergency room or hospital.
This article is republished from The Conversation under a Creative Commons license. Read the original article.![]()