New universal platform for cancer immunotherapy developed
(Medical Xpress) -- Researchers from the Perelman School of Medicine at the University of Pennsylvania report this month in Cancer Research a universal approach to personalized cancer therapy based on T cells. It is the first time a system for making an adaptable, engineered T-cell to attack specific tumor types has been proposed, depending on which abnormal proteins, called antigens, are expressed by individual patients' tumor cells.
For now, the system is being refined in experiments using healthy donor T cells and animal models of human cancer, with the aim to introduce the personalized cells into patients in the future, explains senior author Daniel J. Powell Jr., Ph.D., a research assistant professor of Pathology and Laboratory Medicine with Penn's Ovarian Cancer Research Center.
Tumor antigens are potential targets of an immune response, and identifying which antigens a patient's tumor cells express would be helpful in designing cancer therapy for that individual. Any mutated protein produced in a tumor cell can act as a tumor antigen. Many tumor cells have surface proteins that are inappropriately expressed for the cell type, or are only normally present during embryonic development. Still other tumor cells display cell surface proteins that are rare or absent on the surfaces of healthy cells and are responsible for activating molecular pathways that cause uncontrolled replication of cells. In most cancers, not all patients have tumor cells that express the exact same antigen, and sometimes tumor cells from a single patient can express different antigens. Because of this complexity, it is important to properly choose which antigen to target with cancer therapy.
T cells engineered to express an engineered antigen, called a chimeric antigen receptor (CAR), offer an attractive strategy for targeting antigens and treating cancer, says Powell. CARs are engineered receptors that graft, for example, the portion of a tumor-specific antibody onto an immune cell. This allows the patients' T cells to recognize tumor antigens and kill their tumor cells.
For therapy, a large number of tumor-specific, cancer-fighting CAR T cells can be generated in a specialized lab using patients' own T cells, which are then infused back into them. This approach has shown promising results in patients whose tumors all express the same antigen.
Despite these encouraging findings, currently made CARs have a fixed antigen specificity, which means only one type of tumor antigen can be targeted at a time. Tumor cells that lack that selected antigen can then escape recognition by immune cells and replicate, limiting what might otherwise have been an effective therapy if multiple tumor antigens had been targeted. For this reason, the team sought to make a more generalized receptor framework that is able to produce T cells capable of targeting large panels of known tumor antigens.
To that end, the team developed a new platform from which they could eventually target a variety of tumor antigens, either simultaneously or sequentially. So far, they have engineered T cells against the antigens mesothelin, present on several tumor cell types; epCAM, present on epithelial cell cancers; alpha folate, present on ovarian cancer cells; and, more recently, CD19 on lymphoma cells.
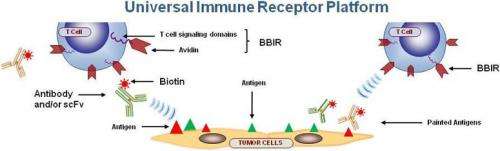
The universal immune receptor recognizes molecules attached to tumor antigens on the surface of tumor cells. When this happens, the T cells produce inflammatory response proteins called cytokines and pore-forming proteins. Those proteins cause the release of enzymes through those pores into tumor cells, thereby killing them.
The new engineered T cells described in the Cancer Research paper recognize and bind exclusively to cancer cells pre-targeted with biotin-labeled molecules, such as antibodies. Biotin is a B complex vitamin necessary for cell growth that can be bound by a molecule called avidin, which is contained in the universal immune receptor. Since nearly any molecule can be biotin labeled, the number of antigens that can be targeted by T cells carrying the biotin-binding immune receptor is nearly infinite. The versatility afforded by this biotin-binding receptor permitted the targeting of a combination of distinct antigens all at once, and even one after another, notes Powell.
The findings demonstrate that a universal T cell can significantly extend conventional CAR approaches, allowing the team to generate T cells of unlimited antigen specificity. This process is geared to make T cell therapy more available to patients and to improve the effectiveness of T-cell immunotherapies for cancer.
First author post-doctoral fellow Katarzyna Urbanska, Ph.D. continues optimization of the universal receptor approach by looking for different ways to improve the interaction of T cells with tumor cells, and how to better direct the T cells and the biotin-labeled molecules to tumor cells in the body.
In the future, Powell and colleagues predict a highly personalized platform for cancer therapy that begins when patient tumors are analyzed for their expression of specific antigens at the Department Pathology and Laboratory Medicine's new Center for Personalized Diagnostics. When the antigens expressed by a patient's tumor cells are determined, their T cells will be engineered to express the universal immune receptor, which will be given back to them in combination with biotin-labeled molecules to attach to patients' tumor antigens for an individualized tumor attack.
More information: cancerres.aacrjournals.org/con … CAN-11-3890.abstract














