Pathophysiology may help ID rare, early form of Alzheimer's
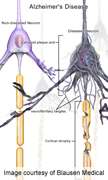
(HealthDay) -- In dominantly inherited Alzheimer's disease, clinical and biomarker changes occur decades before the expected onset of disease symptoms, according to a study published online July 11 in the New England Journal of Medicine.
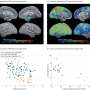
Randall J. Bateman, M.D., from the Washington University School of Medicine in St. Louis, and colleagues conducted a prospective longitudinal study, analyzing data from 128 participants to examine the order and magnitude of pathologic processes. The participants underwent baseline clinical and cognitive assessments, brain imaging, and cerebrospinal fluid (CSF) and blood tests. The participant age at baseline and parental age at the onset of Alzheimer's symptoms were used to estimate the years to symptom onset.
Twenty-five years before expected symptom onset, the researchers found that the concentrations of amyloid-beta (Aβ)42 in the CSF appeared to decline. Fifteen years before expected symptom onset, Aβ deposition in the brain was detected, as were increased concentrations of tau protein in the CSF and an increase in brain atrophy. Ten years before expected symptom onset, cerebral hypometabolism and impaired episodic memory were observed. Five years before expected symptom onset, global cognitive impairment was detected, as measured by the Mini-Mental State Examination and the Clinical Dementia Rating scale. The diagnostic criteria for dementia were met an average of three years after expected onset of symptoms.
"Autosomal dominant Alzheimer's disease was associated with a series of pathophysiological changes over decades in CSF biochemical markers of Alzheimer's disease, brain amyloid deposition, and brain metabolism as well as progressive cognitive impairment," the authors write.
Several authors disclosed financial ties to pharmaceutical, biotechnology, and diagnostic companies.
More information:
Abstract
Full Text
Copyright © 2012 HealthDay. All rights reserved.