Gene mutation study results could lead to less expensive, more accessible breast and ovarian cancer screening
(Medical Xpress)—Researchers conducting a study of gene mutations that increase a woman's likelihood of breast and ovarian cancers have made a discovery that could open doors to less expensive and more accessible breast and ovarian cancer screening. Additionally, the surprising study results may also explain how human embryos with these breast cancer mutations survive.
The study, recently published by the prestigious online medical journal PLoS ONE, examined the genetic makeup of women who were known carriers of the mutated breast and ovarian cancer susceptibility gene BRCA1 and 2 (BRCA1/2). Women without BRCA1/2 mutations have a lifetime risk of 12% for breast and 1.4% for ovarian cancers. However, with a BRCA1/2 mutation, the risk for breast cancer increases to 60% and for ovarian cancer to 15-40%.
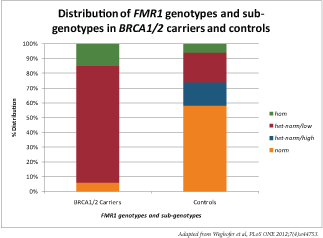
According to the results of the study, conducted by three teams of researchers from the Center for Human Reproduction (CHR) in New York, NY, USA; the Medical University Vienna in Vienna, Austria; and the Medical University Graz, in Graz, Austria; nearly all of the 99 subjects who were carriers of the BRCA1/2 mutations also had a very specific genotype known as "low" FMR1. In contrast, over 300 control subjects, who were not carriers of the mutated BRCA1/2 gene, showed normal distribution of the FMR1 genotypes with only about 25% of the subjects having the "low" FMR1. The authors concluded that because BRCA1/2 mutations are almost exclusively found in women with low FMR1, women without the low FMR1 genotype would not be at risk for BRCA1/2 mutations and, therefore, associated breast and ovarian cancer risks.
This link, according to researchers, suggests that less expensive FMR1 gene testing could be used in place of the current method of the costly BRCA1/2 screening for these cancer risks.
"We were very surprised by these results," said David H. Barad, MD, MS, Director of Clinical ART and Senior Scientist at CHR, a senior author of the study. "This observation, if confirmed, can greatly impact current cancer screening methods for BRCA1/2-associated cancers in women, and greatly reduce costs."
Currently, the only available genetic screening for breast and ovarian cancers is through the testing of the BRCA1/2 gene. However, due to the unusually high costs of the tests (about $3,000), testing is only recommended for women with a strong family history of these cancers. FMR1 testing, on the other hand, is available for as little as $400.
The authors note that the most likely explanation for why so many women with the BRCA1/2 mutation also have low FMR1 genotypes is that the BRCA1/2 mutation is lethal to human embryos; only those embryos carrying a low FMR1 in addition to the BRC1/2 mutation survive, apparently rescued by the presence of a low FMR1 allele.
Further Study Implications: Solving the BRCA-paradox
The published report also notes that these findings may also help explain the mystery of the "BRCA-paradox," which has puzzled researchers for years. This paradox refers to the fact that BRCA1/2 mutation prevents cell growth and replication in embryonic tissue – making it lethal to a growing human embryo. However, in cancerous tissues, these mutations have exactly the opposite effect, allowing cancer cells to proliferate.
"Confirmed, these findings could mean that 'low' FMR1 alleles de-suppress the anti-proliferative activity of BRCA1/2 in both tissues, in embryonic tissues allowing the embryo to survive, while in cancers having the negative effect of allowing cancer to proliferate," explains Norbert Gleicher, MD, Medical Director and Chief Scientist of CHR, and another senior author of the study. "This, of course, could open major therapeutic options for improving embryo growth and inhibiting cancer growth."
More information: Weghofer et al, BRCA1/2 mutations appear embryo-lethal unless rescued by low (CGG n<26) FMR1 sub-genotypes: Explanation for the "BRCA paradox"? PLoS ONE 2012; dx.plos.org/10.1371/journal.pone.0044753
"BRCA1 and BRCA2: Cancer Risk and Genetic Testing." National Cancer Institute at the National Institutes of Health. www.cancer.gov/cancertopics/factsheet/Risk/BRCA. 7 September 2012.