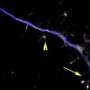
A fly mutation suggests a new route for tackling ALS
A team of researchers, led by Marc Freeman, PhD, an early career scientist with the Howard Hughes Medical Institute and associate professor of neurobiology at the University of Massachusetts Medical School have discovered a gene in the fruit fly Drosophila melanogaster that, when mutant, blocks the self-destruction of damaged axons, which could hold clues to treating motor neuron diseases, such as amyotrophic lateral sclerosis (ALS).
A neuron has a very distinctive form – a bush of dendrites that receive signals, an incredibly long axon, which is like a long tail, and "a little dot" between them that is the cell body, housing the genetic headquarters. Every part of the neuron is required for it to transmit messages. "If anything breaks along any part of the neuron, the cell unplugs from the circuit and no longer functions," explained Dr. Freeman, who presented this research at the Genetics Society of America's 54th Annual Drosophila Research Conference in Washington, D.C.
Once the long tail-like axon is damaged, it shrivels away, basically self-destructing, and resulting in neurons that no longer operate. This catastrophic damage can happen in several ways: from inflammation, a neurodegenerative disease, a metabolic disorder such as diabetes, toxin exposure, or tumor growth. Such axon loss is thought to be a primary factor that leads to functional loss in patients with neurological disorders – it is equivalent to going into an electrical circuit and randomly cutting wires.
The study of axon destruction in response to damage goes back to British neurophysiologist Augustus Waller, who in 1850 described how an axon separated from the cell body and cut off from its nutrient supply breaks apart and is dismantled by scavenger cells. "The idea that this process, called Wallerian degeneration, was a passive wasting away of the axon held for 150 years," Dr. Freeman said.
Then in the late 1980s, researchers discovered a mutation in the mouse, called Wlds, which enables a damaged axon to survive for weeks after injury. "That fundamentally changed how we think about an axon. Under certain circumstances, axons can survive for a much longer time than we have given them credit for," Dr. Freeman explained.
Freeman's laboratory speculated that if axon self-destruction is an active process, then there should be genes in the fly genome whose normal function is to destroy cut axons. They decided if they could break those genes responsible for axon destruction, then the axons shouldn't fall apart. To identify those genes, they performed a labor-intensive screen, randomly breaking genes in the fly genome and looking for those that when broken blocked axon destruction after injury.
This approach led to the identification of one gene, called dSarm, whose normal function is to promote the destruction of the axon after injury. "We got beautiful protection of axons when we knocked out this molecule," Dr. Freeman said. Mice and humans have forms of this gene too, and Freeman and colleagues have shown its functions in a similar way in mice. The preservation of these signaling mechanisms from flies to humans is a sign of evolutionary retention and argues for its importance.
To get closer to applying the axon death gene to the study of disease, the researchers crossed the mouse version of the Sarm mutation into a mouse model that has a type of familial ALS, which is also in humans. Although the mice still lost weight and had difficulty with a mobility test, they lived about 10 days longer than their brethren without the Sarm mutation, and at least half of their motor neurons remained intact. "Since not all the motor neurons are needed," Dr. Freeman said, "even with a 50 percent reduction a patient could feel very close to normal. It would be life-changing for the patient, so it's a step in the right direction."
"We used Wallerian degeneration as a model for axon degeneration. We've identified a signal pathway whose normal function is to promote axon destruction after injury, and hope to build on this research to better understand the role of axon death in neurodegenerative diseases," Dr. Freeman summed up.










.jpg)