Study uncovers gene's contribution to asthma susceptibility
New research from the University of Minnesota College of Veterinary Medicine (CVM) has uncovered the role gene ORMDL3 plays in the disease asthma. ORMDL3, a gene recently linked to asthma susceptibility, has now been linked to the body's ability to recruit inflammatory cells during an airway allergic reaction. Study findings appear today in the journal Nature Communications.
U of M researchers including Srirama Rao, Ph.D., (P. Sriramarao), CVM professor in the Department of Veterinary and Biomedical Sciences and associate dean for research, as well as professor in the U of M Medical School's Division of Pulmonary, Allergy, Critical Care and Sleep Medicine, has identified a function of how ORMDL3 regulates the recruitment of inflammatory cells to airways, thus causing airway inflammation, in a mouse model.
Sung Gil Ha, Ph.D., a CVM post-doctoral fellow and the study's lead author, and colleagues have identified factors that up-regulate the ORMDL3 gene in specific white blood cells such as eosinophils during allergic asthma. Eosinophils are white blood cells intended to help protect the body from parasites; however, in the case of certain types of inflammation including exposure to allergens, instead of providing protection, they can cause tissue damage leading to asthma or other allergic disorders.
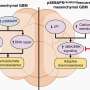
Not much is known about the function of ORMDL3 in asthma. By silencing or over-expressing ORMDL3 in eosinophils, the group has identified molecules regulated by the gene. These molecules enable eosinophils to congregate in airways where they cause allergic inflammation.
When turning the ORMDL3 gene off, researchers found lower levels of integrins expressed on the surface of eosinophils, meaning a decreased ability of eosinophils to migrate and cause inflammation in the airways.
"While exciting, our finding is just one piece of the puzzle," said Rao. "The more we understand about various asthma susceptibility genes including ORMDL3, the better positioned we will be to strategize new treatment options."
The discovery provides momentum for future understanding of the pathogenesis of asthma and role of genetics in inflammatory allergic reactions. This research is not only relevant for asthma but potentially other allergic disorders such as those of the GI tract and skin. The American Academy of Allergy, Asthma & Immunology estimates the number of asthma suffers internationally at 300 million with 250,000 annual deaths attributed to the disease.
Genetic disposition can influence the severity or susceptibility to an asthmatic reaction to allergens or environmental factors such as stress and cold.
The ORMDL3 gene studied by U of M researchers has been linked to asthma in various ethnic groups worldwide.