Clinical study finds 'bubble CPAP' boosts neonatal survival rates
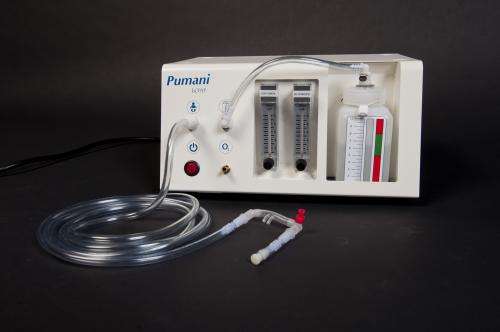
The first clinical study of a low-cost neonatal breathing system created by Rice University bioengineering students demonstrated that the device increased the survival rate of newborns with severe respiratory illness from 44 percent to 71 percent.
The results, which were published online this week in the open-access journal PLOS ONE, came from a 10-month study of 87 patients at Queen Elizabeth Central Hospital (QECH) in Blantyre, Malawi. Based on data from the study, it is estimated that treatment with low-cost "bubble CPAP" could save the lives of 178,000 low-birth-weight babies in Africa each year.
The researchers found that premature infants with complications like sepsis, very low birth weight and respiratory distress syndrome (RDS) benefited most from the new technology. Survival rates more than doubled for babies with RDS and more than tripled for babies in the other two categories after treatment with bubble CPAP. The technology is a low-cost version of the continuous positive airway pressure (CPAP) systems that are a standard feature of most neonatal units in the developed world.
"Premature birth is now the second leading cause of death among children worldwide, and most premature babies are born in low-resource settings where many of the basic technologies and approaches that lead to improved outcomes are unavailable," said Dr. Elizabeth Molyneux, a pediatrician at QECH, who co-authored the report with colleagues from Rice, QECH, Baylor College of Medicine, and the University of Malawi. "The results from the bubble CPAP clinical study are dramatic, and thanks to the partnership of QECH, Rice and the Malawi Ministry of Health, we are already implementing bubble CPAP nationwide."
CPAP helps babies breathe more easily by keeping their lungs inflated, but with a price around $6,000, conventional neonatal CPAP machines are too expensive for hospitals in the developing world. In 2010, a team of Rice bioengineering students invented a low-cost bubble CPAP device. The technology, which costs about 15 times less than conventional CPAP machines, was created as part the Rice 360°: Institute for Global Health Technologies' award-winning, hands-on engineering education program, Beyond Traditional Borders (BTB).
QECH, the main referral hospital in southern Malawi, admits about 3,000 babies per year to its neonatal ward. The 2012 clinical study involved newborns suffering from respiratory distress. Patients were treated with bubble CPAP whenever a machine and trained staff were available. The study included data from 62 infants who were treated with bubble CPAP and a control group of 25 infants who received nasal oxygen from an oxygen concentrator, the current standard of care in Malawi.
The survival rate for babies treated with bubble CPAP was 71 percent, compared with 44 percent for the control group. The survival rates for infants with the following complications were also much higher if the babies were treated with bubble CPAP: respiratory distress syndrome, 64 percent with bubble CPAP compared with 23 percent without; very low birth weight, 65 percent with bubble CPAP compared with 15 percent without; and sepsis, 61 percent with bubble CPAP and zero without.
"The improvement that we saw for premature babies with respiratory distress syndrome mirrored the improvement that was seen in the United States when CPAP was first introduced here," said Rice's Rebecca Richards-Kortum, the Stanley C. Moore Professor and chair of the Department of Bioengineering and director of both BTB and Rice 360°.
Respiratory distress claims the lives of about 1 million African newborns each year. Based on the dramatic results from the study, QECH, Rice 360° and the Malawi Ministry of Health have partnered to provide bubble CPAP at all 27 of the country's government hospitals. To date, 22 of the machines have been installed at nine hospitals, and 354 clinicians have been trained to use them.

Richards-Kortum and Maria Oden, director of Rice's Oshman Engineering Design Kitchen (OEDK), founded the hands-on BTB engineering education program in 2006. BTB sends about a dozen Rice students overseas each summer to work with partners and test design prototypes—like bubble CPAP in 2010—that Rice students have created throughout the school year at the OEDK.
QECH has hosted BTB students each summer since 2006, and Richards-Kortum and Oden raised $375,000 in donations this year for the Day One Project, an ambitious effort to expand QECH's neonatal facilities and to establish an "innovation hub" at the hospital where student-developed technologies can be proven and showcased.
"It's difficult to overstate the importance of the clinical results for bubble CPAP," said Oden, a co-author of the new study. "Not only have we shown that this specific technology can save thousands of lives each year, we've also demonstrated a technology pipeline that can produce many similar technologies in the future."
Through the Day One Project, Rice 360° and QECH hope to create a collection of low-cost neonatal technologies that an African district hospital serving 250,000 people can implement for about $5,000.
Additional pilot programs for bubble CPAP are set to begin this year at teaching hospitals in Tanzania, Zambia and South Africa, thanks to a $400,000 prize announced Nov. 14 as part of the inaugural Healthcare Innovation Award program sponsored by pharmaceutical giant GlaxoSmithKline and London-based nonprofit Save the Children. A group led by QECH's charitable arm, Friends of Sick Children in Malawi, won the competition's top prize with its proposal to replicate the success of Malawi's bubble CPAP program in three neighboring countries.
In September, bubble CPAP was chosen by the United Nations as one of 10 "Breakthrough Innovations That Can Save Women and Children Now." Thanks to the designation from the UN's Every Woman, Every Child program, the technology was displayed for the U.N. General Assembly Sept. 23 as part of an effort to mobilize governments, multilaterals, the private sector and civil society to address the major health challenges facing women and children around the world.

















