Diabetes researchers track cells' ability to regenerate

Vanderbilt University scientists have found evidence that the insulin-secreting beta cells of the pancreas, which are either killed or become dysfunctional in the two main forms of diabetes, have the capacity to regenerate.
The surprising finding, posted online recently by Cell Metabolism, suggests that by understanding how regeneration occurs, scientists one day may be able to stop or reverse the rising tide of diabetes, which currently affects more than 8 percent of the U.S. population.
The study "provides clues to how we might learn what signals promote beta-cell regeneration in type 1 and type 2 diabetes," said Alvin Powers, M.D., the paper's senior author and director of the Vanderbilt Diabetes Center.
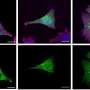
In the past three months, the Powers group at Vanderbilt, in four separate papers, has reported important findings about the "microenvironment" of the insulin-secreting beta cells and glucagon-secreting alpha cells, which are among four types of cells clustered in "islets" in the pancreas.
Both hormones are important in regulating blood glucose levels and ensuring that glucose is delivered to muscles and brain to be burned as fuel, and stored in the liver. Powers called the islets a "mini-organ" because they are highly vascularized and innervated, and exist within a specialized environment.
In type 1 diabetes, the beta cells are destroyed and glucose levels rise in the blood because not enough insulin is being produced. In type 2 diabetes, a frequent consequence of obesity, tissues become resistant to insulin, again causing blood glucose to rise. Beta cell function also becomes abnormal.
Marcela Brissova, Ph.D., research assistant professor of Medicine, was first or co-first author on three of the manuscripts. Chunhua Dai, M.D., research assistant professor of Medicine; and Kristie Aamodt and Rachel Reinert, Ph.D., students in the Vanderbilt M.D./Ph.D. program, were also among the first or co-first authors.
In two papers in the journal Diabetes and one each in Development and Cell Metabolism, the researchers described four main findings about islet vascularization and innervation:
First, vascular endothelial growth factor A (VEGF-A) is important for development of the islets' blood supply and for beta-cell proliferation. Blocking the growth factor early in development in a mouse model ultimately reduced beta-cell mass and insulin release and impaired glucose clearance from the bloodstream.
Other Vanderbilt scientists involved in this work were postdoctoral fellow Fong Cheng Pan, Ph.D., and Owen McGuinness, Ph.D., professor of Molecular Physiology and Biophysics.
Second, VEGF and other "signals" released by the endothelial cells lining islet blood vessels consequently stimulated growth of islet nerves in mice that connected to the brain.
"If the islets don't become vascularized properly, they don't become innervated properly," Brissova said. These signals also promote beta cell growth.
Other Vanderbilt scientists involved in this research were Ambra Pozzi, Ph.D., professor of Medicine, and Christopher V.E. Wright, D.Phil., Louise B. McGavock Professor, Department of Cell and Developmental Biology.
Third, VEGF-A was not involved when the beta-cell mass increased in an obese mouse model of type 2 diabetes in response to rising glucose levels.
Unlike tumors, which sprout new blood vessels as they grow, the beta-cell tissue increased its blood supply by dilating existing vessels.
Other Vanderbilt scientists involved in this research were Takamune Takahashi, M.D., Ph.D., associate professor of Medicine; Masakazu Shiota, DVM, Ph.D., associate professor of Molecular Physiology and Biophysics; and Eric H. Liu, M.D., assistant professor of Surgery.
Finally, too much VEGF-A can lead to beta cell death. But that sets up a regenerative microenvironment involving an interaction of vascular endothelial cells and macrophages which, in turn, leads to beta cell proliferation both in mice and human islets.
"That's very, very unusual because islet cells are like neurons; once they're dead, they don't usually regrow," Brissova said. "We think that the endothelial cells and macrophages which are recruited from the bone marrow create an environment that promotes the proliferation and regeneration of those beta cells."