Mystery of the pandemic flu virus of 1918 solved
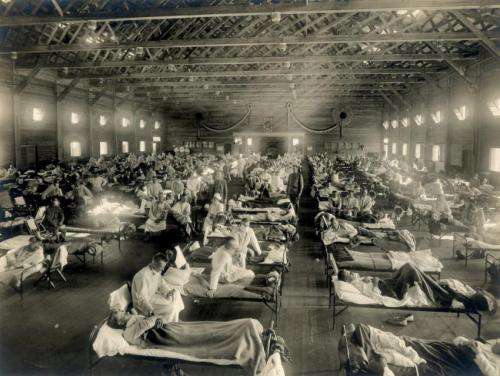
A study led by Michael Worobey at the University of Arizona in Tucson provides the most conclusive answers yet to two of the world's foremost biomedical mysteries of the past century: the origin of the 1918 pandemic flu virus and its unusual severity, which resulted in a death toll of approximately 50 million people.
Worobey's paper on the flu, to be published in the early edition of the Proceedings of the National Academy of Sciences (PNAS) on April 28, not only sheds light on the devastating 1918 pandemic, but also suggests that the types of flu viruses to which people were exposed during childhood may predict how susceptible they are to future strains, which could inform vaccination strategies and pandemic prevention and preparedness.
"Ever since the great flu pandemic of 1918, it has been a mystery where that virus came from and why it was so severe, and in particular, why it killed young adults in the prime of life," said Worobey, a professor in the UA Department of Ecology and Evolutionary Biology. "It has been a huge question what the ingredients for that calamity were, and whether we should expect the same thing to happen tomorrow, or whether there was something special about that situation."
Worobey and his colleagues developed an unprecedentedly accurate molecular clock approach and used it to reconstruct the origins of the 1918 pandemic H1N1 influenza A virus (IAV), the classical swine H1N1 influenza virus and the post-pandemic seasonal H1N1 lineage that circulated from 1918 until 1957. Surprisingly, they found no evidence for either of the prevailing hypotheses for the origin of the 1918 virus – that it jumped directly from birds or involved the swapping of genes between existing human and swine influenza strains. Instead, the researchers inferred that the pandemic virus arose shortly before 1918 upon the acquisition of genetic material from a bird flu virus by an already circulating human H1 virus – one that had likely entered the human population 10-15 years prior to 1918.
"It sounds like a modest little detail, but it may be the missing piece of the puzzle," Worobey said. "Once you have that clue, many other lines of evidence that have been around since 1918 fall into place."
If these individuals had been already been exposed to an H1 virus, it could explain why they experienced much lower rates of death in 1918 than those who died in greatest numbers, a cohort centered on those about 29 years of age in 1918.
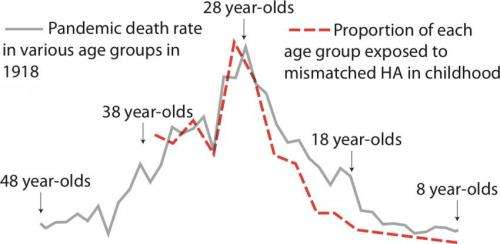
IAV typically kills primarily infants and the elderly, but the pandemic virus caused extensive mortality in those ages 20 to 40, primarily from secondary bacterial infections, especially pneumonia. The authors suggest that this is likely to be because many young adults born from about 1880 to 1900 were exposed during childhood to a putative H3N8 virus circulating in the population, which featured surface proteins distinct to both the major antigenic proteins of the H1N1 virus.
The authors compared the virus' genetic history with the types of antibodies present in people from different generations alive in 1918 and with death-by-birth-year patterns not only in 1918 but also in later years. The combined lines of evidence suggest that this small wedge of the population may have been uniquely susceptible to severe disease in 1918, whereas most individuals born earlier or later than between 1880 and 1900 would have had better protection against the 1918 H1N1 virus due to childhood exposure to N1 and/or H1-related antigens.
The authors speculate that long-term protection, for example the perplexingly low mortality in very elderly people in 1918 who may have been exposed in youth to an H1N1-like virus, might be mediated by immune responses to relatively slowly evolving regions of the viral HA protein.
"Imagine a soccer ball studded with lollipops," Worobey explained. "The candy part of the lollipop is the globular part of the HA protein, and that is by far the most potent part of the flu virus against which our immune system can make antibodies. If antibodies cover all the lollipop heads, the virus can't even infect you."
The part of the protein that represents the stem of the lollipop in this analogy is less exposed to the immune system's responses.
"Antibodies binding the HA stalk might not prevent infection altogether, but they can get in the way enough to prevent the virus from multiplying as much as it otherwise would, which protects you from severe disease and death," Worobey said.
"But a person with an antibody arsenal directed against the H3 protein would not have fared well when faced with flu viruses studded with H1 protein," Worobey said, "And we believe that that mismatch may have resulted in the heightened mortality in the age group that happened to be in their late 20s during the 1918 pandemic."
The authors note that childhood exposure to mismatched viral proteins may nevertheless have been better than nothing: isolated populations on islands where many individuals might have had no prior exposure to IAV before 1918 suffered mortality rates many times higher than the "H3N8" cohort of young adults worldwide.
The authors suggest that immunization strategies that mimic the often impressive protection provided by initial childhood exposure to influenza virus variants encountered later in life might dramatically reduce mortality due to both seasonal and novel IAV strains.
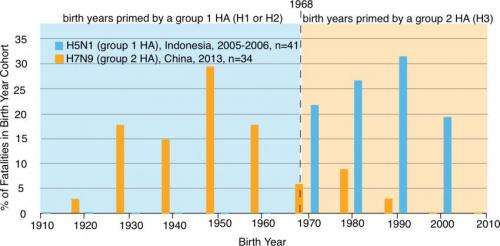
Worobey said the new perspective does not just apply to the pandemic of 1918, but might also explain patterns of seasonal flu mortality and the mysterious patterns of mortality from highly pathogenic avian origin H5N1. H5N1causes higher mortality rates in young people and H7N9 causes higher mortality in the elderly. In both cases, the more susceptible age groups were exposed initially, as children, to viruses with a mismatched HA, and may suffer severe consequences similar to young adults faced with a mismatched virus in 1918.
"What seems to be the decisive factor is prior immunity," Worobey said. "Our study takes a variety of observations that have been difficult to explain and reconciles and places them into a logical chain able to explain many patterns of influenza mortality over the last 200 years. What we need to do now is to attempt to validate these hypotheses and determine the exact mechanisms involved, then apply that knowledge directly to better prevent people from dying from seasonal flu and future pandemic strains."
More information: Genesis and pathogenesis of the 1918 pandemic H1N1 influenza A virus, PNAS, www.pnas.org/cgi/doi/10.1073/pnas.1324197111