Experimental heart attack drug reduces tissue damage, minimizes bleeding risk
(Medical Xpress)—An investigational drug studied in animals significantly reduced damage to heart muscle from a heart attack and minimized the risk of bleeding during follow-up treatments, according to a study by scientists at Washington University School of Medicine in St. Louis.
"This medication, known as APT102, has the potential to change the paradigm for how heart attack patients initially are treated," said senior author Dana Abendschein, PhD, associate professor of medicine and of cell biology and physiology at Washington University. "This also may be a better way to treat strokes caused by or associated with a blood clot."
The study, which was funded by a National Institutes of Health (NIH) Small Business Innovation Research Grant and by APT Therapeutics Inc., the developer of APT102, is available online in Science Translational Medicine.
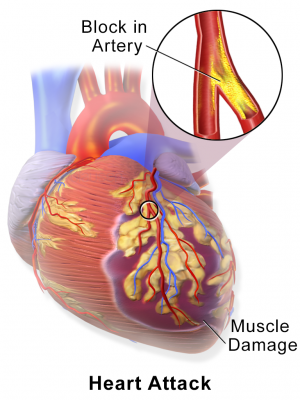
Standard heart attack treatment often causes heart tissue damage. Once the blood clot that causes a heart attack is removed from an artery, molecules from dead and dying cells mix with blood rushing back through the artery. One of these molecules, adenosine triphosphate (ATP), is inflammatory; another, adenosine diphosphate (ADP), causes more clotting.
"ATP and ADP have different roles, but they both lead to more heart damage as they flood through the reopened artery after a heart attack," said Abendschein.
The experimental drug APT102 is a genetically engineered version of the human protein apyrase, which transforms ATP and ADP into a benign molecule, adenosine monophosphate. Another enzyme changes this molecule into adenosine, which is beneficial for the heart.
"Adenosine opens the blood vessels, increases blood flow and also has a protective effect on the lining of the vessels," said Abendschein. "It takes the bad products away and produces a good byproduct that's protective."
The scientists treated 21 dogs for the study. After the clots that caused their heart attacks were dissolved using medication, eight received the standard post heart-attack drug clopidogrel, a blood thinner; seven were given low doses of APT102; and six were given high doses of APT102.
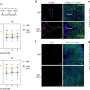
The researchers found that treatment with APT102 significantly reduced the amount of irreversible heart muscle damage.
"That's a huge benefit because the majority of patients who have a lot of heart muscle damage go on to have heart failure," Abendschein said.
By breaking down the clotting factor ADP, treatment with APT102 also eliminated the return of the clots, which can lead to further heart damage.
"Virtually every agent that's being used in patients now to prevent clot formation blocks the blood clotting agents known as platelets, and that creates a risk of bleeding," Abendschein said. "This is not true of APT102."
Other anticlotting agents have to be digested and converted into their active form in the liver, but APT102 can be injected directly into a vein, where it works immediately.
"When it comes to heart attack treatment, the saying is 'time is muscle'—the longer you delay treatment, the more irreversible damage the heart will suffer," Abendschein said. "APT102 may help us save critical time by letting treatment start right away."
Abendschein and his team at Washington University have worked with APT Therapeutics and researchers at Harvard and Cornell over the past 10 years to develop the data published in Science Translational Medicine. They hope to start clinical trials of the drug in people within the next year.
More information: Moeckel D, Jeong SS, Sun X, Broekman MJ, Nguyen A, Drosopoulos JHF, Marcus AJ, Robson SC, Chen R, Abendschein D. Optimizing human apyrase to treat arterial thrombosis and limit reperfusion injury without increasing bleeding risk. Science Translational Medicine, online Aug. 6, 2014.