Breast cancer cells recycle to escape death by hormonal therapy

Many breast cancer cells facing potentially lethal antiestrogen therapy recycle to survive, researchers say.
About 70 percent of breast cancer cells have receptors for the hormone estrogen, which acts as a nutrient and stimulates their growth. Patients typically get an antiestrogen such as tamoxifen for five years to try to starve them to death, says Dr. Patricia V. Schoenlein, cancer researcher in the Medical College of Georgia Schools of Medicine and Graduate Studies.
"About 50 to 60 percent of these women really benefit from hormonal therapy," says Dr. Schoenlein. Why others don't has been asked for at least two decades.
One reason may be breast cancer cells switch into a survival mode that normal cells also use when faced with starvation, according to research published in the September issue of Molecular Cancer Therapeutics. Dr. Schoenlein also is reporting on the research during the 2nd World Conference on Magic Bullets (Ehrlich II) Oct. 3-5 in Nürenberg, Germany.
It's called macroautophagy – autophagy means "self eating" – and within a week, breast cancer cells can reorganize component parts, degrade non-essentials and live in this state until antiestrogen therapy is stopped or the cells mutate and resume proliferation in the presence of tamoxifen. "It's like taking your foot off of the gas pedal of your car," says Dr. Schoenlein, corresponding author on the study. "The cancer cell is in idle, unable to grow or replicate. But the cell is smart enough to use component parts generated by macroautophagy for the most necessary things required for survival." She notes that macroautophagy can't be maintained indefinitely; cells can actually self-digest. "This is a time-buying strategy."
Chemotherapeutic drugs are more direct killers but also kill healthy cells and can be tolerated by patients only for relatively short periods. Antiestrogen therapy is more specific, targeting breast cancer cells that express estrogen receptors.
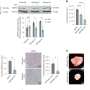
In the laboratory, 20-25 percent of breast cancer cells died when Dr. Schoenlein and colleagues gave antiestrogen continuously over time – similar to how patients get it. More typically, the cells expressed increasing levels of macroautophagy and survived. "They don't grow, but they survive the therapy. They will grow if you take away the therapy." Adding a macroautophagy inhibitor promoted robust cell death.
"We believe targeting the autophagosome function will significantly improve the efficacy of hormonal treatment for estrogen-positive breast cancer," says the researcher. She recently received a three-year, $1.1 million National Cancer Institute grant to pursue that strategy.
She'll now look for ways to block macroautophagy in an animal model, including using chloroquine, a drug used to treat malaria. "We know patients can take it with few side effects," she says. If it works in animals, the drug, in combination with an antiestrogen, could move relatively quickly into human testing.
During autophagy, the internal pH for the recycling center of the reorganized cell gets acidic and chloroquine increases pH. "If you add this particular inhibitor of the recycling center, you alter the pH and block its ability to do what it is supposed to do," says Dr. Schoenlein.
A University of Pennsylvania team led by Dr. Craig Thompson reported in 2007 in The Journal of Clinical Investigation that chloroquine increased death of suicide-resistant lymphoma cells being treated with chemotherapy. Dr. Schoenlein will give chloroquine along with an antiestrogen and measure cell death.
"Most cancers probably use autophagy as a survival mechanism. You can either block the autophagosome with your therapy or you can make the cell eat itself to the point of no return and the cell self-destructs. You have to push it either way," she says. Although there are no known compounds in clinical use to induce self-destruction by autophagy, there is some evidence arsenic trioxide, a compound used in China to treat some aggressive cancers, prompts cancer cells to die from self digestion, she says. That and other compounds will no doubt be studied further, she says.
Dr. Schoenlein believes breast cancer survival during macroautophagy requires high activity of the tumor suppressor protein Rb and low levels of the lipid ceramide. Ceramide is vital but causes cell death at high levels. MCG researcher Erhard Bieberich and colleague Dr. Brian G. Condie at the University of Georgia showed in 2003 that high levels of ceramide kill cells that are unnecessary to the developing brain. The new studies will further explore the roles of Rb and ceramide in breast cancer survival during macroautophagy and determine if chloroquine can change their balance.
Source: Medical College of Georgia