Fluorescent co-enzyme is an early indicator for breast cancer
(PhysOrg.com) -- Think back to high-school biology and you may recall some basics about cellular respiration: how organelles called mitochondria function like little power stations, converting nutrients from food into a high-powered cell fuel called adenosine triphosphate, or ATP.
ATP powers the activity of every cell -- and every living thing -- on Earth. Yet without a key coenzyme called nicotinamide adenine dinucleotide (NADH), ATP could not be made.
NADH is aglow with good press these days for its potential use in helping cancer specialists differentiate between healthy and cancerous cells, especially in early disease stages.
Penn State associate professor of bioengineering, Ahmed Heikal, and his graduate student Qianru Yu, have made two intriguing discoveries about this enzyme. They pioneered a method for measuring NADH levels in living cells and then determined that NADH molecules, which are naturally fluorescent, are twice as prevalent in breast cancer cells as they are in normal breast cells, a trait that could serve as an indicator of easily-missed early-stage malignancies.
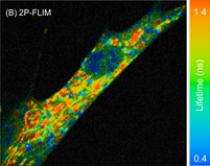
Using a combination of microscopy and state-of-the-art spectroscopy, Heikal and Yu have found a way to convert NADH’s fluorescence into an accurate measure of its concentration in live cells, as a means of analyzing whether a cell’s metabolic and respiratory processes are healthy or damaged.
Normal cells are aerobic, Heikal said. Inside healthy mitochondria, both oxygen and NADH are essential to convert energy from nutrients into ATP. But some cancer cells (those in tumors, for example) are anaerobic. Their mitochondria are disabled, causing the voracious, rapidly-dividing malignant cells to use a faster form of metabolism -- gylcolysis -- to turn sugar into energy without using oxygen. During this process, Heikal said, “the concentration of NADH inside these diseased cells increases.”
Heikal and Yu’s method of testing intracellular NADH levels offers several advantages over existing approaches.
“Conventional techniques require cell destruction,” said Heikal. “Studying living cells, non-invasively and under physiological conditions, is important because it allows us to understand how they function under diseased conditions. We can measure real-time dynamic changes with high spatial resolution as the cells respond to external stimulation from drugs, mechanical stress, or viral infection.”
One challenge that remains to be overcome, Heikal and Yu said, is that their technique uses ultrashort infrared laser, which penetrates only a fraction of a millimeter into biological tissues.
“This inherently limits our ability to monitor mitochondrial activities and NADH concentration deep in human tissues or organs,” Heikal said.
He predicts that new non-linear, fiber-based imaging techniques currently being developed in research laboratories around the world will provide the solution. If and when they do, the potential of this diagnostic tool “is limitless in both basic and applied research as well as in clinical setting,” Heikal said. “Our quantitative and non-invasive approach would be ideal in helping to diagnose a wide range of diseases,” including neurodegenerative conditions such as Alzheimer’s and Parkinson’s diseases, as well as cancer, and even aging. The same approach, he said, could be applied to study other fundamental questions in cell and molecular biology.
Provided by Pennsylvania State University (news : web)















