New mechanism explains how the body prevents formation of blood vessels
Researchers at Uppsala University, in collaboration with colleagues in Sweden and abroad, have identified an entirely new mechanism by which a specific protein in the body inhibits formation of new blood vessels. Inhibiting the formation of new blood vessels is an important aspect of, for example, cancer treatment. The study is published in the November issue of the journal Molecular Cancer Research.
Angiogenesis, the formation of new blood vessels, is strictly regulated by a number of molecules that serve to either promote or inhibit the process. Certain diseases are characterised by excessive or insufficient angiogenesis. The rapid growth of tumors, for example, is conditioned on the formation of new blood vessels to supply oxygen and nutrients, which explains why angiogenesis is accelerated in cancer patients.
"At present, there are five approved drugs for inhibiting formation of new blood vessels," says research fellow Anna-Karin Olsson of the Department of Medical Biochemistry and Microbiology at Uppsala University, who headed the study. "All of these medications work in a similar way, by influencing the function of one of the agents that promotes angiogenesis. A problem with the medications is that the body develops resistance to them as treatment progresses. Improved knowledge about which molecules promote or inhibit the formation of blood vessels in the body, and the mechanisms by which they operate, is accordingly a research goal."
The study in question involved researchers from Uppsala University collaborating with colleagues in Sweden, Norway, Finland and Germany to investigate the function of histidine-rich glycoprotein (HRG), a plasma protein naturally present in the body. Previous studies involving mice had shown that HRG inhibits angiogenesis and tumor growth. The new study demonstrates, among other things, that the HRG fragment responsible for the inhibitory effect is present in human tissue, which suggests that it serves as one of the body's own angiogenesis inhibitors.
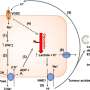
The HRG fragment in question inhibits angiogenesis by binding to endothelial cells, which participate in the formation of blood vessels. Analysis of a large number of human tissue samples allowed the researchers to determine that the HRG fragment binds to blood vessels in cancer patients but not in healthy persons. The study also showed that the HRG fragment binds to blood vessels in the presence of activated platelets, blood cells that limit bleeding in the event of injury. This finding is interesting in view of the fact that cancer patients often exhibit high levels of platelet activation.
"Our findings suggest that attempting to inhibit angiogenesis is an aspect of the body's own reaction to diseases like cancer," says Anna-Karin Olsson. "The activated platelets create a microenvironment in which the HRG fragment is able to function as an angiogenesis inhibitor."
Data from so-called "knockout" mice, which lack HRG, support this conclusion. The mice are healthy and fertile, but exhibit high levels of angiogenesis in connection with tumor growth. This finding is consistent with the hypothesis that the mice lack an angiogenesis inhibitor.
"Our data describes an entirely new mechanism of action for an endogenous angiogenesis inhibitor," says Anna-Karin Olsson. "This knowledge may eventually help in developing new, more effective drugs for inhibiting angiogenesis during disease treatment without affecting healthy vessels."
Source: Uppsala University (news : web)