New patented technology for improving cardiac CTs receives NIH support
Cardiovascular disease is the leading cause of death globally and a tremendous burden on the healthcare system. Better detection of hardening or clogging of arteries and other blood vessels before symptoms occur is needed.
With funding from the National Institutes for Health (NIH), researchers from Virginia Tech and GE Global Research Center are developing novel cardiac computed tomography (CT) architectures and methods, including a newly patented approach to a long-standing challenge in local CT image reconstruction (Patent 7,697,658 "Interior Tomography and Instant Tomography by Reconstruction from Truncated Limited-angle Projection Data" issued April 13, 2010). The research team will also evaluate the performance of various cardiac CT system designs to determine the most promising designs and demonstrate their clinical feasibility and utility.
Better image quality at lower radiation dose is the immediate need being addressed by the research project led by Ge Wang, the Pritchard Professor and director of the Biomedical Imaging Division of the Virginia Tech - Wake Forest University School of Biomedical Engineering & Sciences (SBES), and Bruno De Man, a CT authority at GE Global Research Center.
Faster, dynamic imaging to capture the beating heart and algorithms or computations that can present the most exact images from X-ray projections are also among project goals. "Cardiac CT technology needs major improvements to capture a fast beating heart with better clarity at lower risk," said Wang.
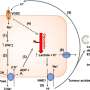
In traditional X-ray CT imaging, data is recorded behind the patient. Everything is superimposed along the X-ray path through the patient. In other words, an X-ray projection of the heart includes the bone and muscle along the way to the detectors. With current CT, the X-rays probe the patient along multiple wide beams focused on the patient including a region of interest, such as the heart, from various orientations. That is, the source of the X-rays rotate around the individual as he or she lies inside a large aperture, then a computer program reconstructs images from the exposures. This CT process increases radiation exposure but generates a lot of different views to be analyzed by physicians for diagnosis.
In many cases, like cardiac CT, the area of interest is just a relatively small region within the larger body. "It was realized long before that one could reduce the radiation dose by sending X-rays just through the region of interest from different directions, and then reconstruct that region from resultant local data," said Wang.
Depending upon the algorithm used, the resulting images can, to different degrees, portray sharp borders or edges from tissue or bone within the region of interest but cannot show X-ray linear attenuation coefficients accurately. "This has been known for decades as the 'interior problem'," said Wang.
A method known as lambda tomography addresses the interior problem by producing changes in the density of the image. "However, physicians need quantitative images, and hence lambda tomography has not been clinically used," said Wang.
His group at Virginia Tech, in collaboration with Professor Yangbo Ye at the University of Iowa, developed the now patented "interior tomography" method for interior reconstruction of a region of interest image to replace lambda tomography. "We assume a known sub-region within the region of interest - such as an air gap, a blood area, or an implant in the heart. With a known sub-region, we can solve the interior problem in a theoretically exact and mathematically stable fashion - we can produce an accurate image!" said Wang.
Interior tomography is a theoretical breakthrough, and Wang and colleagues as well as peer groups have been developing it and publishing results. The patent application was filed in 2007. The proof of concept was an important basis for the aforementioned NIH grant.
"We have been using different mathematics to reconstruct the images on a region of interest and have compared the results to the conventional CT images reconstructed from a so-called "complete dataset," which was acquired with wide beams of X-rays, and not truncated. It becomes clear that interior tomography has practical implications," said Wang. "We have data that shows its promise. While medical CT can presently only perform global image reconstruction, we look forward to having precise local reconstruction from a highly truncated dataset."
By applying interior tomography to medical CT, radiation exposure can be reduced, and a large patient can be accommodated because the focus will be on the region of interest and not the entire body.
A scheme is also being developed for faster imaging based on interior tomography (Medical Physics, Vol. 36, No. 8, August 2009). "Cardiac motion limits image quality, but of course you want the heart to be beating," said Wang.
Hardware solutions consist of multi-source imaging, examples of which have already been introduced, including a dual-source cone-beam scanner from Siemens just three years ago. "However, the bulkiness of the detectors and limited space inside a CT gantry still make it impossible to collect a large number of projections simultaneously," Wang said. "And it is expensive and cannot accommodate a large patient."
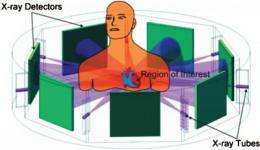
His group proposes a multisource interior tomography concept. For example, the individual is surrounded by a half dozen or more X-ray tubes and detectors. X-rays are focused in narrow beams on the region of interest and the detectors are also small, not requiring much room. More than 10 views per second are possible, and interior tomography software can potentially provide accurate images of the beating heart.
A greater challenge occurs when physicians introduce an unknown agent into the image field. "Introducing contrast material complicates the situation," said Wang. "The material alters blood density in unpredictable ways. Contrast material disperses quickly as the heart beats and physicians want to see that happen, so we are working to improve interior tomography to create image results without precise sub-region knowledge."
The solution by Hengyong Yu, the associate director of the CT laboratory at Virginia Tech; Jiansheng Yang and Ming Jiang of Peking University; and Wang is based on compressed sensing, a mathematical method for reducing the number of unknowns based on some sparsity model (Yu and Wang: Physics in Medicine and Biology, vol. 54, number 9 (2009), 2791). "Among all the images that are possible solutions, we select that with the minimum variation and have proved that this approach would give the unique solution assuming the image being piece-constant or piece-polynomial. Reconstruction for interior tomography thus could do the job even if we do not have precise knowledge on a sub-region. That is a promising direction we are working along," said Wang.
Co-PIs on the NIH project are Yu with Wang's group; Kai Zeng, electrical engineer at GE Global Research Center; Hao Lai, manager of the GE Global Research CT and X-ray systems and applications laboratory; and Darin Okerlund, manager of GE Healthcare's applications engineering team.
The patented approach to interior tomography and instant tomography by reconstruction from truncated limited angle projection data was developed by Wang, Ye, and Yu. Virginia Tech Intellectual Properties Inc. has filed numerous patent applications for inventions by Wang's team, most of which improve the performance of biomedical imaging. Research has been funded by the National Institute of Biomedical Imaging and Bioengineering, National Cancer Institute, National Heart, Lung and Blood Institute, National Science Foundation, and other funding agencies.
Wang has collaborated with GE Global Research for a number of years. The company, based in Niskayuna, NY, is a world leader in medical equipment development and manufacturing. "It has critical technologies to the proposed program," said Wang. "In addition, GE's healthcare business integration will ensure successful transfer of improved technologies into the market place for the benefit of patients."
Wang said that he expects that the cardiac CT systems and methods identified by the NIH-funded project will significantly improve diagnostic performance and therapeutic outcomes.