Scientists reveal how genetic mutations may cause type 1 diabetes
Scientists from The Scripps Research Institute have provided an answer to the 40-year-old mystery of how certain genetic mutations lead to Type 1 diabetes. This new molecular understanding could lead to novel therapies for Type 1 diabetes and other autoimmune diseases.
The study was published in an advanced, online issue of the Journal of Clinical Investigation on April 19, 2010, and will appear in the May print edition of the journal.
"People have been looking for the mechanism linking HLA and autoimmunity for 40 years," said Scripps Research Professor Luc Teyton, who led the study with Scripps Research Professor Ian Wilson. "This study provides a big leap forward in understanding and suggests a critical new target to intervene in type 1 diabetes."
Teyton notes that his lab has been trying to solve the mystery of autoimmune mechanisms and related conditions like celiac disease for some 25 years.
A Life-Threatening Condition
This new study focuses on Type 1, or insulin-dependent diabetes, a rapidly progressive disease of the young that leads to high blood sugar, coma, and death if not treated with replacement insulin.
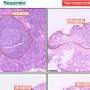
Type 1 diabetes occurs when the body's immune system attacks insulin-producing β cells in the pancreas. Without insulin, the glucose in the bloodstream increases dramatically; early symptoms are unusual thirst, increased output of urine, fatigue, and unusual hunger accompanied by weight loss.
Currently, the only therapy available is to compensate for the destruction of the body's insulin-producing cells by injecting insulin on an ongoing basis.
While genes predispose people to many different types of diseases in many different ways, specific genetic variations are an especially strong predictor of the development of type 1 diabetes. Three genetic variations in particular (HLA-DQ2, HLA-DQ8, and HLA-DR0405)—all located in the region of the genome called HLA for "human leukocyte antigen"—are known to dramatically increase risk of coming down with the condition.
These three genes encode molecules that present peptides (protein fragments) to the body's T cells. T cells then determine whether the peptide being presented is dangerous and needs to be eliminated from the body—as in the case of foreign invaders such as bacteria or viruses—or whether the peptide is "self," part of the host and something the immune system needs to leave alone. However, in the context of type 1 diabetes, T cells aggressively attack the body's own cells.
The scientists wanted to know on a molecular level how mutations in the immune surveillance machinery could lead to type 1 diabetes.
"We were interested in trying to understand why certain MHC molecules (which are molecules in mice analogous to HLA molecules in humans) are linked to autoimmune disease, particularly type 1 diabetes," said Research Associate Adam Corper of the Wilson lab, who was first author of the paper with Kenji Yoshida of the Teyton lab. "In particular, we wanted to know why a single residue at position 57 on the β chain of HLA molecules seems to be linked to the disease."
Breaking Tolerance
In the new research, the team used a series of structural and biophysical studies to answer that question.
Previously, Teyton and Wilson labs had determined the structure of a "diabetogenic" MHC molecule and found that mutations to position 57 caused only subtle changes. It did not, as some had speculated, cause the molecule to become unstable and non-functional.
Now, in the new study the researchers found that diabetes-causing mutations changed the charge at one end of the MHC peptide-binding groove. In individuals not predisposed to type 1diabetes, MHC molecules usually have a negatively charged residue at position 57. In contrast, disease-causing MHC molecules have a neutral residue at position 57 and consequently the surrounding region is more positively charged.
The result of this molecular change was that the mutated MHC molecules selected a unique subset of T cells that bound to it strongly, with "higher affinity." These T cells may overreact and potentially misidentify "self" peptides as dangerous rather than harmless.
"We found that the MHC region around position 57 can be seen by the T cell receptor," said Teyton. "That's the big novelty of the paper—for the first time, we show that it is not only essential for peptide binding, but also critical for the selection of T cells. Finally, we have an idea of why those particular MHC molecules are associated with disease."
Corper added, "What we have here is potentially a way of breaking 'tolerance'—the mechanism where the immune system doesn't respond to self. Obviously, if that breaks down you get autoimmune disease."
The team is now investigating potential antibody or small molecule therapies that could target and correct mutated MHC.