Study identifies new therapies for prevention and treatment of Alzheimer's disease
A Blanchette Rockefeller Neurosciences Institute (BRNI) study published today in the Journal of Neuroscience reveals underlying causes for the degeneration of synapses in Alzheimer's Disease and identifies promising pharmaceutical solutions for the devastating condition that affects more than 5 million people in the United States. The BRNI study is the first to achieve fundamental molecular understanding of how synapses are lost in Alzheimer's Disease before the plaques and tangles develop. At the same time, it is the first study to demonstrate the comprehensive benefits of synaptogenic compounds in treating Alzheimer's Disease.
The BRNI study marks an important shift in our understanding of how Alzheimer's Disease is caused and should be treated. Previous autopsy-based studies have shown the critical role of synaptic loss in producing dementia (though, not the reason behind the degeneration), yet for decades scientists and pharmaceutical companies have focused on ways to target the amyloid plaques and neurofibrillary tangles thought to play a role in causing Alzheimer's Disease. By preventing the loss of synapses, BRNI's new therapeutics prevent the progressive symptoms of Alzheimer's Disease.
"Alzheimer's Disease is not primarily a disease of plaques and tangles as many had previously concluded, it is most importantly a disease of synapses," said Dr. Daniel Alkon, the scientific director of BRNI and co-author of the study, "This study found that treatments that target the loss of synapses in the Alzheimer's brain, can virtually eliminate all other elements of the disease – elevation of the toxic protein, A Beta, the loss of neurons, the appearance of plaques, and loss of cognitive function; the animals' brains were normalized."
The study utilized mice genetically engineered to express the symptoms and pathology of human Alzheimer's Disease in two different strains. BRNI used a difficult training regimen for the mice in order to reveal that significant cognitive deficits occurred five months before plaques were detected in their brains, providing evidence that plaques and tangles are not at the root of the disease.
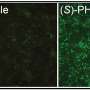
Treatments of Bryostatin and similar compounds synthesized at BRNI that target the enzyme PKCε, which controls the creation of synapses at the molecular level, were administered for twelve weeks during the study. While the compounds promoted the growth of new synapses and preservation of existing synapses, they also stopped the decrease of PKCε and the increase of soluble β amyloid, meaning that the treatments could be used to prevent the familiar hallmarks of Alzheimer's Disease, the plaques and tangles. BRNI has received approval to move forward with Phase II clinical testing for Bryostatin to treat Alzheimer's Disease, which is set to begin within the next several months.
The synaptogenic BRNI drugs have also shown potential for the treatment of traumatic brain injury (TBI), as recently reported in the journal Neurobiology of Disease, and stroke described in the Proceedings of the National Academy of Science in 2008 and 2009.
The target of the synaptogenic compounds is the same molecule identified as a biomarker for early diagnosis of Alzheimer's Disease in clinical trials conducted by BRNI and published in Neurobiology of Aging in 2010. As a result of that study, researchers at the Institute are now working to develop a skin test for identifying Alzheimer's Disease in its early stages before significant progression.