Drug treatment shows promise for brain blood vessel abnormality
A drug treatment has been proven to prevent lesions from cerebral cavernous malformation -- a brain blood vessel abnormality that can cause bleeding, epilepsy and stroke -- for the first time in a new study.
The drug fasudil, which prevented the formation of lesions in a genetic mouse model of the disease, shows potential as a valuable new tool in addressing a clinical problem that is currently treatable only with complex surgery.
"The results are very exciting because they represent the first-ever evidence of a drug effect on the development of cavernous angiomas in living animals," said Issam Awad, MD, professor of surgery at the University of Chicago Medical Center and senior author of the study appearing in the journal Stroke. "The result was very dramatic. The prevalence of lesions went down significantly, and the lesions that developed in the mice were simpler and smaller and did not show any inflammation or bleeding."
Cerebral cavernous malformation (CCM), also known as cavernous angioma, occurs when small blood vessels of the brain grow abnormally large and irregular. The walls of these blood vessels can become stretched and thin, occasionally leaking blood into the brain and leading to hemorrhages, seizures, vision or hearing problems, and strokes.
CCM is estimated to occur in one out of 200 people, though the lesions may not always cause symptoms. Currently, when a CCM lesion is detected in an MRI of a patient, the only option is to wait and see whether it grows large enough to require brain surgery, Awad said.
"There is currently no treatment in clinical use to either prevent the formation or the maturation of these lesions," Awad said. "The way we deal with them now is we wait until a lesion gets bad or does something bad, and then we take it out."
Roughly one-third of CCM cases result from hereditary, familial forms of the disease, the most common of which was traced to a gene called CCM1 or KRIT1. By reducing this gene's activity, Awad's team in Chicago and geneticist Douglas A. Marchuk's team at Duke University successfully created CCM lesions in living mice. This model replicated familial CCM and allowed the testing of new treatments to prevent or reverse lesions.
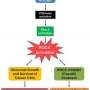
In a parallel collaboration with Mark H. Ginsberg's group at the University of California, San Diego, the researchers proved that knocking down the CCM1 gene resulted in elevated activity of a signal called ROCK, which can make brain blood vessels "leaky." Further studies found that CCM lesion tissues resected from human patients and the mouse model also exhibited abnormally high ROCK activity. In light of these results, the researchers at the three institutions hypothesized that treatment with a drug inhibitor of ROCK might prevent CCM lesions from forming and rupturing.
Fasudil is the only specific ROCK inhibitor drug available for animal studies and human use, and has been tested for treatment of conditions such as angina and pulmonary hypertension. In the Stroke paper, first author David McDonald and colleagues tested whether a long-term treatment with fasudil could prevent lesion formation in CCM model mice.
After four months of treatment, genetically modified mice given fasudil displayed fewer and less severe lesions and fewer signs of hemorrhage and inflammation than similar mice given placebo treatment.
"This animal model and humans have lesions that are aggressive and symptomatic: They leak blood, they show inflammatory properties, and endothelial cells multiply or proliferate," Awad said. "None of these features were present in the fasudil-treated mice. It was like the lesion was chilled down and shrunk."
Fasudil is approved for clinical use in Japan for the treatment of a condition called cerebral vasospasm after aneurysm rupture, and it has been clinically well tolerated for that indication. In the U.S., the drug is not currently approved but has been tested in clinical trials for angina and pulmonary hypertension. If future experiments continue to support its effectiveness in CCM, Awad and colleagues hope to work with the drug manufacturers and the United States Food and Drug Administration to move this therapy to human clinical trials.
"This treatment approach will require validation and optimization in additional experiments before initiation of clinical trials; nevertheless, no other drug has ever before been shown to prevent lesion development, and this effect appears very promising," Awad said. "Our collaborative group is uniquely positioned with tools in hand to help develop this therapy."
Awad and colleagues are also hopeful that fasudil treatment might benefit sporadic forms of CCM, where they have detected increased ROCK activity. In the meantime, the fasudil results in mice offer hope that neurologists may soon have a preventative treatment that can ease the worries of patients with familial CCM.
"This treatment does not cure the disease," Awad said. "But if it is successfully translated to human therapy, it would be a bit like treating multiple sclerosis, where many treatments do not eliminate the primary disease trigger, but can muffle it, slow it down and make it not as serious, and therefore allow a patient to effectively live with the disease, as opposed to having the disease dictate their health."
More information: The paper, "Fasudil decreases lesion burden in a murine model of cerebral cavernous malformation disease," will be published online Oct. 27, 2011, by Stroke, and in the January 2012 print issue of the journal.