Overlooked nighttime spikes on EEGs may reflect an underlying brain injury
Children with developmental delay or autism may have unrecognized epilepsy-like brain activity during sleep, report researchers at Boston Children’s Hospital. These nighttime electrical spikes, detectable only on EEGs, occur even in some children without known epilepsy and appear to result from early strokes or other early life injuries to the developing brain, the study found. Results were published online April 25 by the journal Neurology.
“Kids can have an almost normal EEG while awake, but may show increased spikes during sleep,” says lead investigator Tobias Loddenkemper, MD, a neurologist in the Epilepsy Center at Boston Children’s. “If nighttime spiking remains undiagnosed and untreated, it may interfere with learning and development. This has been frequently overlooked in the past.”
Based on their findings, the researchers suggest that sleep EEG monitoring should be considered more often in children not meeting developmental milestones, and that bedtime medications to suppress nighttime seizures may be beneficial if heightened brain electrical activity is found. In a preliminary treatment trial, such nighttime dosing before times of greatest spike or seizure activity has been found to be beneficial.
The study involved sleep EEG monitoring in 147 patients who were suspected of having excess brain electrical activity during sleep, based on loss of developmental milestones, and, in some cases, known seizures. All children had at least one brain MRI available for review. The EEGs and MRIs were read by physicians who did not know details of the patients’ history.
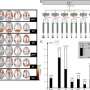
Of the 147 patients, seen at Boston Children’s over a 14-year period, 100 had prominent EEG spikes during sleep; the other 47 (controls) did not. Although there was no significant difference between groups in the percentage of patients with recognized seizures (78 percent of the “spike” group versus 64 percent of controls) or on most clinical measures, the “spike” group had significantly more patients with brain lesions on MRI (48 vs. 19 percent).
Children with EEG spikes were especially more likely than controls (14 vs. 2 percent) to have damage in the thalamus, the structure that relays sensory and motor signals to the cortex and regulates sleep and consciousness. The most common type of brain injury was early stroke (found in 14 vs. 0 percent, respectively).
The authors speculate that these early injuries disrupt circuit formation in the developing brain and lead to over-excitability – too much communication that is reflected in the EEG spikes and that may impinge on learning and development. “We know that children lose skills when these spikes appear,” says Loddenkemper. “These children lose out on a critical period of brain development and may never fully catch up later in life.”
Loddenkemper notes that up to 20 percent of children with heightened nighttime brain electrical activity do not have seizures or recognizable epilepsy. “Developmental delay may be the only clinical finding in some children,” he says. “Children at age 2 or 3, and sometimes older, may suddenly lose developmental milestones such as language, walking skills or fine motor movement.”
In the future, Loddenkemper and colleagues hope to conduct a prospective, multicenter trial in which they follow children with known early brain injury and monitor their nighttime EEG activity. They will then try different drugs to suppress nighttime spiking to see how the children’s long-term learning and development are affected.
Iván Sánchez Fernández, MD, of Boston Children’s Hospital and Universidad de Barcelona (Spain) was first author on the paper. There was no outside funding for the study.