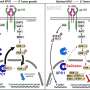
Fertility drug usage and cancer risk
Women using fertility drugs who did not conceive a 10-plus week pregnancy were at a statistically significant reduced risk of breast cancer compared to nonusers; however, women using the drugs who conceived a 10-plus week pregnancy had a statistically significant increased risk of breast cancer compared to unsuccessfully treated women, but a comparable risk to nonusers, according to a study published July 6 in the Journal of The National Cancer Institute.
Ovulation-stimulating fertility drugs temporarily elevate estrogen levels in women, and estrogen is known to play an important role in breast cancer. While some studies report increased breast cancer risk following infertility treatment, other analyses have been inconclusive.
In order to determine the risk of young-onset breast cancer after use of ovulation-stimulating fertility drugs, Chunyuan Fei, Ph.D., at the National Institute of Environmental Health Sciences (NIEHS), and colleagues, conducted a sister-matched case-control study, in part funded by Susan Komen for the Cure, called the Two Sister Study (which was developed from the Sister Study), which looked at women diagnosed with breast cancer under the age of 50 years and their breast cancer-free control sisters, who were studied between September 2008-December 2010. They looked specifically at fertility-drug exposure according to whether or not it had resulted in a pregnancy lasting at least 10 weeks.
The researchers found that women who had used fertility drugs showed a non-statistically significantly reduced risk of breast cancer compared to women who did not use fertility drugs and women who used fertility drugs and did not conceive a 10-plus week pregnancy were at a statistically significantly lowered risk of breast cancer compared to nonusers. Women who had used fertility drugs and conceived a 10-plus week pregnancy did, however, have a statistically significantly increased risk of breast cancer compared to women who had been unsuccessfully treated. "Our data suggest that exposure to a stimulated pregnancy is enough to undo the reduction in risk associated with a history of exposure to ovulation-stimulating drugs," the authors write. They believe the exposure to the fertility drugs potentially raises risk by modifying pregnancy-related remodeling of breast tissue. However, successfully treated women had a comparable level of breast cancer risk to non-users.
The authors note a few limitations of the study, including the reliance on self-reported fertility drug usage, and lack of data on specific diagnosis for infertility.
In an accompanying editorial, Louise A. Brinton, Ph.D., of the Division of Cancer Epidemiology and Genetics at the National Cancer Institute, feels that the findings of the study are hard to understand in the context of previous studies with results ranging from a lowered risk to a higher risk to no relationship between the drugs and the risk of early onset of breast cancer. Brinton explains that the reduced overall risk associated with drug usage may be related to the fact that one of the drugs, clomiphene, is a selective estrogen receptor modulator (SERM) similar to tamoxifen, an established chemo-preventative. On the other hand, increased risk seen in successfully treated women may be related to the increased exposure to ovarian hormones, as well as "the dual effect of pregnancy on breast cancer risk, namely a short-term transient increase that dissipates with time and eventually leads to a long-term risk reduction," Brinton writes. Another complicating factor in interpreting the study's results is its focus on women who developed breast cancer before age 50, which is more often associated with genetic factors than breast cancers diagnosed at a later age.
Brinton concludes that additional research is needed to understand these associations. "Because of such complexities, results from individual investigations must be cautiously interpreted and weighed against the considerable benefits associated with fertility drug usage, including a high probability of carrying pregnancies to term, which can lead to substantial long-term reductions in breast cancer risks."