Anti-cancer drug fights immune reaction in some infants with Pompe disease
Adding a third anti-cancer agent to a current drug cocktail appears to have contributed to dramatic improvement in three infants with the most severe form of Pompe disease—a rare, often-fatal genetic disorder characterized by low or no production of an enzyme crucial to survival.
Duke researchers previously pioneered the development of the first effective treatment for Pompe disease via enzyme replacement therapy (ERT). ERT relies on a manufactured enzyme/protein to act as a substitute for the enzyme known to be lacking in patients with a particular disease. In Pompe disease, ERT has been found to reduce heart and muscle damage caused by the absence of the enzyme.
In the new study, appearing online in the Oct. 11, 2012, edition of the journal Genetics in Medicine, the Duke team added a new step to the therapeutic regimen to address complications suffered by a subset of infants with Pompe disease who are treated with ERT. Some infants with Pompe disease who have certain combinations of genetic mutations develop a severe immune response to ERT. Very high levels of antibodies become directed against the enzyme and greatly reduce its therapeutic effect, leading to rapid clinical decline and death.
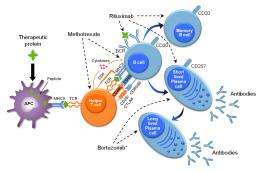
In a January 2012 publication in Genetics in Medicine, the researchers reported success in preventing the immune rejection in Pompe infants who were just beginning ERT. They treated them with a drug cocktail that included low doses of the cancer chemotherapy drugs rituximab and methotrexate, plus the immune booster gammaglobulin to prevent the immune response to the ERT.
The three cases described in the new paper had already received the ERT for a prolonged period of time and, despite initial improvements, declined rapidly as their bodies developed high levels of antibodies that blocked the effect of the enzyme replacement. In these youngsters, plasma cells, which are the ultimate source of antibody production, were left untouched by the immune-suppressing drug cocktails.
"These plasma cells form rapidly after exposure to ERT, and some of them are what we call long-lived plasma cells that survive for years, continuing to spew out antibodies," explained senior author Priya Kishnani, M.D., professor of Pediatrics and Medical Genetics at Duke.
After testing their ideas in mouse models of Pompe disease, the Duke researchers added a proteasome inhibitor called bortezomib to the regimen. Bortezomib, which is FDA-approved to treat multiple myeloma and mantle cell lymphoma, targets the plasma cells and inhibits the production of antibodies, reversing the established immune response.
In all three cases the antibodies decreased rapidly. Just as rapidly, each of the babies' conditions dramatically improved and the babies have continued to do well.
"I'm absolutely delighted, because to me this has become life-saving for these fragile babies," Kishnani said. "This is what I truly think is translational research, where you learn about a problem in patients, address it in an animal model and take it back into the patients to make a difference."
"We were encouraged with the positive results from preclinical studies using bortezomib. We quickly developed a clinical protocol using bortezomib for infantile Pompe patients that had failed conventional treatment. It was truly a satisfying experience," said first author Suhrad Banugaria, MBBS, postdoctoral associate in Pediatrics Medical Genetics at Duke.
Next, the group is working to develop treatments that more specifically target antigens eliciting immune responses to ERT. Kishnani and colleagues hope that such a targeted approach might minimize the impact on the immune system generally.
Kishnani said the insights her team has gained treating Pompe disease could be applied to other diseases in which an immune response has also been shown to reduce the impact of enzyme replacement therapy.
"We're already getting calls for other conditions such as mucopolysaccharidosis and Fabry disease, where physicians are facing the same issues: patients who have developed a significant antibody response and are not doing as well, or have started to show a clinical decline," Kishnani said.















