Beating new life into a heart transplant

Human hearts which are not used each year because they are deemed unsuitable for an organ transplant could get a second chance to save a life, with the help of new research taking place in the North East.
Organ shortage is one of the most pressing issues concerning the field of transplantation,with hundreds of Britons a year dying while on the transplant waiting list, and coronary heart disease being one of the biggest killers in the UK.
From potential donors, some hearts are not retrieved due to their unsuitability for organ transplantation. Now new research at the University of Sunderland to restart hearts and develop tests to prove they are still viable, could potentially use more of the declined donor hearts, potentially helping to reduce transplant waiting lists.
As a result of successful pre-clinical tests in the lab to get dead pigs' hearts beating once again, clinical trials are to begin on human hearts that would not otherwise have been used after ethical approval was granted by National Research Ethics service in Newcastle. The research work has also been done in collaboration with Newcastle University.
Dr Noel Carter, senior lecturer in molecular biology at the University of Sunderland's Faculty of Applied Sciences, explained: "We have demonstrated enough evidence in our results from restarting pigs' hearts after several hours of being clinically dead, to be able to begin clinical testing on human hearts that are considered too marginal to be used for transplant or as a source of heart valves.
"Heart surgeons have to be 100 per cent positive that this vital organ is going to work before transplantation, which is why a number of them end up not being used. Our research wants to take those rejected hearts, get them restarted, carry out echocardiograms and tests in a sterile environment to check activity and show them to be in perfect working order. We believe then a proportion could be reconsidered for transplantation."
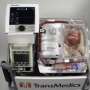
The research team has developed a novel circulatory equipment and defibrillators to pump warm, oxygenated blood through the hearts and used dialysis to filter out unwanted products from the circuit thereby restoring the heart's metabolic activity.
Dr Carter added: "We are devising a series of parameters to test the hearts and ensure that they would be viable if a transplant goes ahead. We believe this could offer new hope for patients and see a greater increase in heart transplants."
Also collaborating on the research is Professor David Talbot, Dr Guy MacGowan, Mr Stephen Clarke and Professor John Dark who all work at Newcastle's Freeman Hospital.
The work is the research project of University of Sunderland PhD student Omar Mownah, a clinical fellow and trainee surgeon, and Susan Stamp, research technician from Newcastle University.
Professor Talbot said "Heart transplantation rates are dwindling year on year within the UK and abroad. This is partly good news as deaths from head injuries through road traffic accidents have fallen but other organ transplants such as the liver and kidney have managed to increase the use of more marginal and older donors. This is often not possible for the heart due to heart disease and the effect of certain drugs on the heart toward the end of life. As a result patients with cardiac failure are increasingly using mechanical devices to support their own hearts as a definitive treatment rather than them being a bridge until a heart transplant becomes available."
Heart transplant is the only option for patients with end-stage heart failure or irreparable coronary artery disease. During this procedure, doctors replace the ailing heart with a healthy one from a brain dead patient.
NHS Blood and Transplant which is the body responsible for organ donation services within the UK are aware and supportive of this research that is entering clinical testing, which has been announced during National Transplant Week (July 8-14).
Professor James Neuberger, Associate Medical Director at NHS Blood and Transplant said: "Surgeons are very keen to transplant every donated organ that can be transplanted safely and will retrieve every organ that might be transplanted in order to ensure that no opportunity is lost. Each donor organ is different and the condition of a heart cannot be fully assessed until it is retrieved.
"We welcome this study and any development that not only increases the quality of organs available for transplant, but also allows those organs currently deemed unsuitable to become of sufficient quality to be transplanted. This research is in the early stages and we await the findings with interest."
Permission to carry out the clinical trials has been done through IRAS (Integrated Research Application System) which is a UK-wide system that streamlines the process for applying for permissions and approvals to conduct health and social care research.
This latest research is in addition to previous work by the same Sunderland research group hoping to expand the donor pool by looking at non-heartbeating donors. These are cases where patients have suffered a heart attack either in intensive care, Accident & Emergency or outside the hospital environment, and there has been an extended period of time in which the body is warm and there is no oxygen being supplied to the organs.
One strategy is to remove the organs and store them cold to try and minimise metabolic damage. The other option is to take a warm oxygenated approach called ECMO (Extra-Corporeal Membrane Oxygenation) where warm oxygenated blood is put round the organs while waiting for them to be transplanted.
This research has led to the development of new medical devices to allow the rapid cooling of the organs, which have been approved by the NHS and have been used in clinical practice.