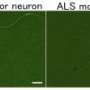
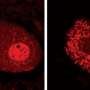
Newly identified bone marrow stem cells reveal markers for ALS
Amyotrophic Lateral Sclerosis (ALS) is a devastating motor neuron disease that rapidly atrophies the muscles, leading to complete paralysis. Despite its high profile—established when it afflicted the New York Yankees' Lou Gehrig—ALS remains a disease that scientists are unable to predict, prevent, or cure.
Although several genetic ALS mutations have been identified, they only apply to a small number of cases. The ongoing challenge is to identify the mechanisms behind the non-genetic form of the disease and draw useful comparisons with the genetic forms.
Now, using samples of stem cells derived from the bone marrow of non-genetic ALS patients, Prof. Miguel Weil of Tel Aviv University's Laboratory for Neurodegenerative Diseases and Personalized Medicine in the Department of Cell Research and Immunology and his team of researchers have uncovered four different biomarkers that characterize the non-genetic form of the disease. Each sample shows similar biological abnormalities to four specific genes, and further research could reveal additional commonalities. "Because these genes and their functions are already known, they give us a specific direction for research into non-genetic ALS diagnostics and therapeutics," Prof. Weil says. His initial findings were reported in the journal Disease Markers.
Giving in to stress
To hunt for these biomarkers, Prof. Weil and his colleagues turned to samples of bone marrow collected from ALS patients. Though more difficult to collect than blood, bone marrow's stem cells are easy to isolate and grow in a consistent manner. In the lab, he used these cells as cellular models for the disease. He ultimately discovered that cells from different ALS patients shared the same abnormal characteristics of four different genes that may act as biomarkers of the disease. And because the characteristics appear in tissues that are related to ALS—including in muscle, brain, and spinal cord tissues in mouse models of genetic ALS—they may well be connected to the degenerative process of the disease in humans, he believes.
Searching for the biological significance of these abnormalities, Prof. Weil put the cells under stress, applying toxins to induce the cells' defense mechanisms. Healthy cells will try to fight off threats and often prove quite resilient, but ALS cells were found to be overwhelmingly sensitive to stress, with the vast majority choosing to die rather than fight. Because this is such an ingrained response, it can be used as a feature for drug screening for the disease, he adds.
The hunt for therapeutics
Whether these biomarkers are a cause or consequence of ALS is still unknown. However, this finding remains an important step towards uncovering the mechanisms of the disease. Because these genes have already been identified, it gives scientists a clear direction for future research. In addition, these biomarkers could lead to earlier and more accurate diagnostics.
Next, Prof. Weil plans to use his lab's high-throughput screening facility – which can test thousands of compounds' effects on diseased cells every day – to search for drug candidates with the potential to affect the abnormal expression of these genes or the stress response of ALS cells. A compound that has an impact on these indicators of ALS could be meaningful for treating the disease, he says.
Prof. Weil is the director of the new Cell Screening Facility for Personalized Medicine at TAU. The facility is dedicated to finding potential drugs for rare and Jewish hereditary diseases.