Research identifies potential link between macrophage response and chronic inflammatory disease
Tiny cells which have the ability to trigger the body's immune responses could be crucial to research into a number of chronic medical conditions, scientists have suggested.
Dr Andrew Foey, from Plymouth University, and Professor StJohn Crean, from the University of Central Lancashire, demonstrated the behaviour of macrophage cells may be linked to the remitting and relapsing nature of the gum disease chronic periodontitis (CP).
They now believe further research could potentially identify links between these cells and other inflammatory diseases which occur throughout the body, and say there is a need to examine ways they could be manipulated to benefit the immune system.
Macrophage cells are present in two forms within the human body – with one type being destructive (inflammatory) and the other reparative (anti-inflammatory) – and they are crucial to the body's ability to control infection.
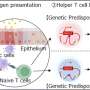
In their current research, published in the PLoS ONE scientific journal, Dr Foey and Professor Crean suggested how CP – a persistent inflammatory condition which, if left untreated, can result in tooth loss – may be impacted by exposure to a particular oral bacteria, Porphyromonas gingivalis, and how macrophage responses were affected by this pathogen.
Dr Foey, Lecturer in Immunology at Plymouth University, said: "We demonstrated that different types of macrophage cell exhibit quite different functional behaviour in response to the bacteria, Porphyromonas gingivalis, upon primary stimulation or re-stimulation. This differential activation or suppression response of macrophage type may go hand-in-hand with the relapsing/remitting presentation of CP and it has been shown that in cases where they over-respond, it can cause uncontrolled inflammation which destroys the soft tissue."
Anti-inflammatory macrophages can be suppressed by persistent oral bacterial stimulation whereas inflammatory macrophages cannot. But this apparent inability of these inflammatory cells to be suppressed by pathogenic bacteria is, Dr Foey suggests, not a wholly negative thing as the body may require some bacterial signals to combat other forms of infection/disease through regulating macrophage responses.
But he added: "Being able to manipulate these cells could impact on a number of conditions which follow a similar behavioural pattern. This highlights the importance of future research endeavours in targeting macrophage cell responses in the treatment of inflammatory diseases."