Mutations during initial infection allows bacteria to evade immune response
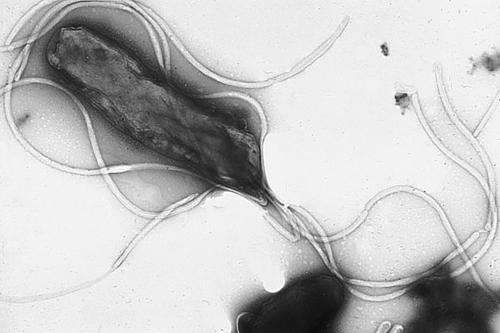
(Medical Xpress)—Bacteria that cause ulcers in humans undergo accelerated evolution during the initial stages of infection, allowing them to evade the immune system, according to new research by an international team of researchers including Penn State scientists. The study shows, for the first time, and in real-time, the interplay between the human immune system and invading bacteria that allows the bacteria to counter the immune response by quickly evolving. A paper describing the research was published in the June 13, 2014 issue of the journal Nature Communications.
"Our next-generation sequencing approach enabled, for the first time, the tracing of Helicobacter pylori infections in human patients," said Stephan Schuster, professor of biochemistry and molecular biology at Penn State.
The scientists compared the genome sequence of the stomach bacterium Helicobacter pylori just prior to infection and at several time points after infection. "We were blown away by the very high mutation rate that we found during the initial phase of infection," said Bodo Linz, research associate at Penn State and lead author of the paper. Patients infected with H. pylori, experience an initial, acute phase of infection during which symptoms are most severe and the immune response is strongest. "We found that the bacteria accumulated mutations at a rate 30 to 50 times faster during this acute phase than during the later, chronic phase of infection when an equilibrium was reached between the bacteria and the immune response," Linz said.
Although the rate at which mutations accumulate in the genome of H. pylori during the chronic phase of infection had been determined previously, no one yet had looked at the initial, acute phase because it is so difficult to capture and sequence the bacteria at the time of initial infection.
To determine the mutation rate during this early phase, the research team took two approaches. First, the researchers isolated the bacteria from two previously-infected human volunteers and determined its genome sequence. After eradicating the bacteria from the volunteers through treatment with antibiotics, they then re-infected the now-cured patients with their own strain of H. pylori. At 20 days after infection in one case and at 44 days after infection in the other, the scientists again isolated the bacteria from the volunteers and sequenced its genome. The patients then received another antibiotic treatment to eliminate the bacteria. "By comparing the genome sequence of the bacteria before and after re-infection, we were able to determine the rate at which the bacterial genome changes during this early, acute phase of infection in a human host," said Linz.
In a parallel experiment, the team infected a rhesus monkey with H. pylori and collected samples of the bacteria from the monkey for genome sequencing at one week, one month, two months, and six months after initial infection. In the monkey, the scientists were able to directly compare the rate of DNA changes in the bacterial genome between the acute and chronic stages. Although mutations continued to accumulate in the bacterial genome during the chronic phase, the rate of substitutions dropped considerably after the initial four-week period.
An infection with H. pylori triggers an immune response that involves the release of reactive oxygen and nitrogen molecules that are known to induce mutations in the DNA sequence and to cause chromosomes to break apart and recombine. Previous studies had shown that the H. pylori genome is forgiving of this kind of abuse. "Strains of the bacterium isolated from different human hosts vary immensely, both in DNA sequence and in gene content" Schuster said. "There are about 1,100 core genes that individual strains of H. pylori share, but another four-to-five-hundred genes vary between strains. The high mutation and recombination rates that produce this variation allow the bacteria to be exquisitely adapted to its host and to evade eradication by the host's immune system."
Of particular importance in the battle between the immune system and invading bacteria are the proteins that protrude through the outer cell membrane of the bacteria. Because these outer-membrane proteins are on the outside of the bacterial cell, they are visible to the human immune system and therefore are targeted by antibodies. "Antibodies are so tuned to recognize the three-dimensional structure of outer-membrane proteins that they can attach to them with lock-and-key specificity, thereby labeling the foreign bacteria cell for elimination," said Linz. Mutations in the genes that code for outer-membrane proteins can produce changes in the protein's structure and, if the key then no longer fits the lock, the genetic mutations allow the bacterium to evade recognition by antibodies. "The intense selective pressure on the bacteria to survive the immune response, coupled with increased mutation rates, produces the incredibly fast rate of genomic change that we discovered in this study," Linz said. "Mutations occur randomly throughout the genome, but because they help the bacteria avoid elimination by the immune system, changes in outer-membrane proteins appear much more often than would be expected by chance in the surviving bacteria."
This initial burst of mutations during the acute phase of infection allows the bacteria to survive the host's immune response and to establish a chronic infection. Whether bacteria other than H. pylori undergo a similar burst of accelerated evolution immediately after infection is not yet known, but the team plans to investigate other common human pathogens in future research.
More information: "A mutation burst during the acute phase of Helicobacter pylori infection in humans and rhesus macaques." Bodo Linz, et al. Nature Communications 5, Article number: 4165 DOI: 10.1038/ncomms5165. Received 19 March 2014 Accepted 20 May 2014 Published 13 June 2014















