Scientists use stem cells to learn how common mutation in Asians affects heart health
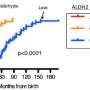
Over 500 million people worldwide carry a genetic mutation that disables a common metabolic protein called ALDH2. The mutation, which predominantly occurs in people of East Asian descent, leads to an increased risk of heart disease and poorer outcomes after a heart attack. It also causes facial flushing when carriers drink alcohol.
Now researchers at the Stanford University School of Medicine have learned for the first time specifically how the mutation affects heart health. They did so by comparing heart muscle cells made from induced pluripotent stem cells, or iPS cells, from people with the mutation versus those without the mutation. IPS cells are created in the laboratory from specialized adult cells like skin. They are "pluripotent," meaning they can be coaxed to become any cell in the body.
"This study is one of the first to show that we can use iPS cells to study ethnic-specific differences among populations," said Joseph Wu, MD, PhD, director of the Stanford Cardiovascular Institute and professor of cardiovascular medicine and of radiology.
"These findings may help us discover new therapeutic paths for heart disease for carriers of this mutation," said Wu. "In the future, I believe we will have banks of iPS cells generated from many different ethnic groups. Drug companies or clinicians can then compare how members of different ethnic groups respond to drugs or diseases, or study how one group might differ from another, or tailor specific drugs to fit particular groups."
The findings are described in a paper that will be published Sept. 24 in Science Translational Medicine. Wu and Daria Mochly-Rosen, PhD, professor of chemical and systems biology, are co-senior authors of the paper, and postdoctoral scholar Antje Ebert, PhD, is the lead author.
ALDH2 and cell death
The study showed that the ALDH2 mutation affects heart health by controlling the survival decisions cells make during times of stress. It is the first time ALDH2, which is involved in many common metabolic processes in cells of all types, has been shown to play a role in cell survival. In particular, ALDH2 activity, or the lack of it, influences whether a cell enters a state of programmed cell death called apoptosis in response to stressful growing conditions.
The use of heart muscle cells derived from iPS cells has opened important doors for scientists because tissue samples can be easily obtained and maintained in the laboratory for study. Until recently, researchers had to confine their studies to genetically engineered mice or to human heart cells obtained through a heart biopsy, an invasive procedure that yields cells which are difficult to keep alive long term in the laboratory.
"People have studied the enzyme ALDH2 for many years in animal models," said Ebert. "But there are many significant differences between mice and humans. Now we can study actual human heart muscle cells, conveniently grown in the lab."
The iPS cells in this study were created from skin samples donated by 10 men, ages 21-22, of East Asian descent.
About 8 percent of the world's population carries the mutation in one of their two copies of the ALDH2 gene, which encodes a protein known as aldehyde dehydrogenase 2. The mutation in the gene short-circuits the production of the functional protein. (Because most carriers have one normal and one mutated copy of the gene, they are not completely lacking in the functional ALDH2 protein.)
One of ALDH2's many jobs in a cell is to seek out and neutralize toxic aldehydes, harmful substances caused by a class of compounds called reactive oxygen species. One toxic aldehyde, called 4HNE, causes the accumulation of yet more reactive oxygen species. Left to their own devices, high levels of reactive oxygen species can signal a cell to undergo programmed cell death in response to stress, such as the lack of oxygen that mimics what happens during a heart attack.
In this study, Ebert and her colleagues first studied the skin cells obtained from the volunteers. Five of the 10 volunteers had an ALDH2 mutation; the other five did not. The researchers found that skin cells with the mutation in the ALDH2 gene had strongly decreased function of the ALDH2 protein compared with the cells without the mutation. The mutated cells also had significantly higher amounts of reactive oxygen species, and grew more slowly than the other cells.
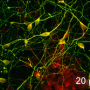
They next created iPS cells from the donated skin samples, and stimulated the iPS cells to become heart muscle cells called cardiomyocytes. They then compared how the newly created cardiomyocytes responded to low-oxygen conditions. Cardiomyocytes with the ALDH2 mutation had higher levels of reactive oxygen species in response to low oxygen levels than those without the mutation, but this difference could be alleviated by treating the cells with a compound that boosts activity of the ALDH2 protein in patients with one unmutated copy of the gene.
Cells with the mutation also were less viable and more likely to undergo programmed cell death than were cells without the mutation. Further study has identified the involvement of a protein called JNK that is activated by high levels of reactive oxygen species. JNK activates a protein called c-Jun known to stimulate programmed cell death.
"This is an entirely new function attributed to this well-known metabolic enzyme," said Ebert. "It's the first time ALDH2 has been shown to play a role in cell survival. Now we have come to understand that when the ALDH2 gene is mutated, cells are more likely to undergo programmed cell death, causing tissue damage."
Establishing biobank of diverse iPS cells
The researchers plan to continue their studies of ALDH2 and its role in maintaining heart health. They would like to investigate further the signaling mechanisms and structural DNA changes that may occur in the presence of the mutation in the ALDH2 gene. This will also allow research on drugs that would increase the activity of the ALDH2 protein in carriers with one good copy and one mutated copy of the gene, which might become a useful therapy for coronary artery disease and heart attacks.
"With our current state of knowledge, it is very likely that we are ignorant of many functions that ALDH2 has in physiological processes," said Ebert.
Wu is working to start a biobank at the Stanford Cardiovascular Institute of iPS cells from about 1,000 people of many different ethnic backgrounds and health histories. "This is one of my main priorities," he said. "For example, in California, we boast one of the most diverse populations on Earth. We'd like to include male and female patients of major representative ethnicities, age ranges and cardiovascular histories. This will allow us to conduct 'clinical trials in a dish' on these cells, a very powerful new approach, to learn which therapies work best for each group. This would help physicians to understand for the first time disease process at a population level through observing these cells as surrogates."
More information: "Characterization of the molecular mechanisms underlying increased ischemic damage in the aldehyde dehydrogenase 2 genetic polymorphism using a human induced pluripotent stem cell model system," by A.D. Ebert, Science Translational Medicine, stm.sciencemag.org/lookup/doi/ … scitranslmed.3009027