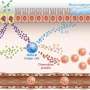
Stem cells derived from amniotic tissues have immunosuppressive properties
Stem cells derived from human amnion have for some time been considered promising for cell therapies because of their ease of access, ability to differentiate, and absence of ethical issues. Now, a Japanese research team has found that stem cells derived from human female amnion also have immunosuppressive activity and that the addition of antibodies to specific factors can enhance their immunosuppressive potential.
The study will be published in a future issue of Cell Transplantation and is currently freely available on-line as an unedited early e-pub.
The amniotic membrane is a tissue of fetal origin comprised of three layers. It is thought that there is a special immunologic mechanism protecting the fetus, so researchers were interested in finding out what immunological properties might reside in - and be extractable from - amnion cells.
"The human amniotic membrane contains both epithelial cells and mesenchymal cells," said study co-author Dr. Toshio Nikaido, Department of Regenerative Medicine, Graduate School of Medicine and Pharmaceutical Sciences at the University of Toyama, Toyoma, Japan. "Both kinds of cells have proliferation and differentiation characteristics, making the amniotic membrane a promising and attractive source for amnion-derived cells for transplantation in regenerative medicine. It is clear that these cells have promise, although the mechanism of their immune modulation remains to be elucidated."
In this study, amnion-derived cells exerted an inhibitory effect on natural killer cells (NKs) and induced white blood cell activation. The researchers reported that the amnion-derived cells saw increases in interleukin-10 (IL-10).
"We consider that IL-10 was involved in the function of amnion-derived cells toward NK cells," explained Dr. Nikaido. "The immunomodulation of amnion-derived cells is a complicated procedure involving many factors, among which IL-10 and prostaglandin E2 (PGE2) play important roles."
Naturally occurring prostaglandins, such as PGE2, have important effects in labor and also stimulate osteoblasts to release factors that stimulate bone resorption by osteoclasts. PGE2 also suppresses T cell receptor signaling and may play a role in resolution of inflammation.
The use of antibodies against PGE2 and IL-10 removed the immunosuppressive effects of the amnion-derived cells by increasing natural killer cell cytotoxicity. This implies that these two factors are contributing elements to the immunosuppressive abilities of amnion-derived cells.
"Soluble factors IL-10 and PGE2 produced by amnion-derived cells may suppress allogenic, or "other" related immune responses," concluded Dr. Nikaido. "Our findings support the hypothesis that these cells have potential therapeutic use. However, further study is needed to identify the detailed mechanisms responsible for their immodulatory effects. Amnion-derived cells must be transplanted into mouse models for further in vivo analysis of their immunosuppressive activity or anti-inflammatory effects."