Study uncovers genetic diversity of pancreatic cancer

A genetic analysis led by UT Southwestern Medical Center researchers suggests that most pancreatic cancers harbor genetic alterations that could be targeted by existing drugs, using their genetic features as a roadmap for treatment. The findings support a precision approach to treating pancreatic cancer, the fourth most deadly cancer for both men and women.
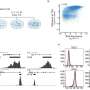
A comprehensive DNA sequencing of pancreatic cancer cases revealed not only a plethora of damaged genes, but potential diagnostic biomarkers that could help identify those with longer or shorter survival, and provide opportunity for new therapeutic interventions. The new findings are published in Nature Communications.
"We identified a wealth of genetic diversity, including multiple mutated genes that were previously unknown to pancreatic cancer ? an important step in gaining a better understanding of this difficult and particularly deadly disease," said lead author Dr. Agnieszka Witkiewicz, Associate Professor of Pathology and a member of the Harold C. Simmons Comprehensive Cancer Center at UT Southwestern. "Importantly, the team was able to identify several genes that may be able to help us to predict outcomes in certain circumstances or serve as good candidates for therapeutic efforts."
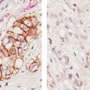
Researchers have long hoped that genetic analysis would provide insight into the biology of pancreatic cancer and define new targets for more effective treatment. Achieving this goal has been hampered by the technical difficulty of isolating pure cancer cells out of the tumor tissue that contains both tumor cells as well as normal cells. The new study overcame this limitation by selectively dissecting cancer cells from pieces of tumor tissue. This method was applied to specifically determine the genetic features of 109 different tumors.
The data showed that the genetic architecture of pancreatic cancer is complex, and each patient's tumor was found to be unique. The genetic features illuminated ways in which the disease arises, defined events associated with survival, and yielded potential targets for therapeutic intervention.
"While we suspect that genetics can be used as the basis of targeted treatments, this point will only be proven through extensive research and clinical studies, hopefully leading to improved outcomes for patients," said senior author Dr. Erik Knudsen, Professor of Pathology, and member of the Simmons Cancer Center who holds the Dr. Charles T. Ashworth Professorship in Pathology. "I am considerably more optimistic of the utility of a genetically targeted therapy for pancreatic cancer today than when we began this work."
Pancreatic cancer is particularly difficult to treat, and is often diagnosed at a late stage when it is no longer amenable to surgical removal. Chemotherapy has a modest effect, and unfortunately the disease progresses in the vast majority of cases. Therefore, new therapeutic regimens are urgently needed.
"Pancreatic cancer will surpass breast and prostate to become the third-leading cause of cancer-related deaths in the next 15 years. If we want to change the death rate, we need to increase the investment in understanding the biology of pancreatic cancer and identifying novel treatment strategies," said co-author and pancreatic cancer surgeon Dr. Michael Choti, Chairman of Surgery, who holds the Hall and Mary Lucile Shannon Distinguished Chair in Surgery.
The study identified a multitude of events that could be selectively targeted in the context of individual pancreatic tumors. For example, the study defined cases of pancreatic cancer that are driven by a gene called BRAF, for which there are FDA-approved drugs, and showed that such drugs were selectively effective against BRAF-mutated pancreatic cancer cells. Similarly, they defined deficits in other features of the tumor cell that can be treated by select drugs.
While these are exciting discoveries for a disease with such a poor prognosis, Dr. Witkiewicz voiced caution.
"Most pancreatic cancers exhibit multiple genetic alterations; therefore, it is likely that combination approaches targeting multiple pathways will be required for effective disease control," she said.