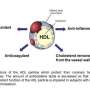
Study links better 'good cholesterol' function with lower risk of later heart disease

HDL is the 'good cholesterol' that helps remove fat from artery walls, reversing the process that leads to heart disease. Yet recent drug trials and genetic studies suggest that simply pushing HDL levels higher doesn't necessarily reduce the risk of heart disease. Now, a team led by scientists from the Perelman School of Medicine at the University of Pennsylvania has shown in a large, forward-looking epidemiological study that a person's HDL function—the efficiency of HDL molecules at removing cholesterol—may be a better measure of coronary heart disease risk and a better target for heart-protecting drugs. Cardiovascular diseases, characterized by the buildup of cholesterol-laden plaques in arteries, currently account for more than 17 million deaths annually, or about a third of the global total.
The scientists found that people whose blood had the highest measures of HDL function at the outset of the study had far fewer heart attacks and other heart disease events in the years that followed, compared to those with the lowest HDL function.
"This is a definitive finding that HDL function, even in people who are still relatively young and healthy, does predict later heart disease events, which implies that therapies that boost HDL function might reduce risk," says senior author Daniel J. Rader, MD, who directs the Preventive Cardiovascular Medicine and Lipid Clinic at Penn Medicine. Rader is also the chair of the department of Genetics.
The new study, reported in the Lancet Diabetes & Endocrinology, used patient data and associated blood serum from a long-running health study in Norfolk, a county in eastern England.
The Norfolk study enrolled more than 25,000 men and women, who had checkups and gave blood samples at an initial visit during 1993 to 1997. Of these people, 1,745 developed coronary heart disease during the follow-up period, which extended to 2009. The team, which also includes first author Danish Saleheen, PhD, an assistant professor of Biostatistics and Epidemiology who performed most of the statistical analyses, used a computer algorithm to select a similarly sized control group, matched for age and other characteristics, from the participants who had no evidence of heart disease during the follow-up period.
The Penn researchers then analyzed the frozen blood samples from the heart disease and control groups to determine their HDL function, termed cholesterol efflux capacity. HDL (high density lipoprotein) molecules in the blood normally assist in the outflow (efflux) of cholesterol from the cholesterol-stuffed macrophage cells in atherosclerotic plaques by taking the macrophages' cholesterol onboard and ferrying it to the liver for excretion in bile. However, one person's HDL may work better at cholesterol removal than another's.
"We don't fully understand why people differ in their HDL cholesterol efflux capacities, but we have known for some time that the size, lipid content, and protein cargo of HDL particles can vary, and there is also some evidence for functional impairment of HDLs in heart disease and diabetes," says Rader.
The team sorted the participants' cholesterol efflux capacities and found that those participants in the top third of efflux capacity scores, compared to those in the lowest third, had 36 percent fewer heart attacks and other indicators of coronary heart disease during the follow up period. That was after adjustments for various confounding factors including age, sex, smoking status, and HDL levels.
Starting with a 2011 paper in the New England Journal of Medicine by Rader's group, researchers have published several epidemiological studies of cholesterol efflux capacity and heart disease. But none of these prior studies has been as large as the new study, or as forward-looking—in fact, most were cross-sectional studies that provided snapshots of efflux capacity and heart disease status at a single point in time.
"I think we now have a convincing story that HDL's ability to promote cholesterol efflux is predictive of future heart disease events even when measured early in a healthy person's life," says Rader.
The large size of the new study also allowed the researchers to find other significant associations within the data. For example, higher cholesterol efflux capacity turned out to be associated with more alcohol intake and fewer cases of diabetes and obesity.
Pharmaceutical companies are still developing drugs to boost HDL levels, and Rader and his colleagues have found in prior studies that some of these compounds also boost HDL cholesterol efflux capacity—an effect that future heart drugs may specifically target. "That's an area of tremendous interest now," Rader says.